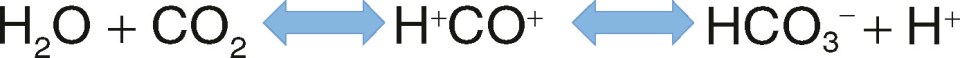Adjustments to sweep gas flow are probably the most common adjustments that you will make in the course of an extracorporeal membrane oxygenation (ECMO) run. While it is entirely feasible that you can go for days on the same blood flow, sweep may need to be adjusted on a daily basis or even multiple times per day.
There is little evidence on optimal strategies for sweep titration and there is significant variation in practice patterns. That said, having a structured approach to adjusting sweep can shape the course of the ECMO run and can optimize management of patients on ECMO. As such, the strategies presented should not be taken as definitive but rather as a proposed approach to the physiologic principles at play.
In general, sweep gas titration is a skill set that gets better with practice. Every adjustment that is made to sweep parameters is an opportunity to assess the clinical impact. As with all critical care interventions, you should have a rationale for changes, estimate the expected result, and then reassess the clinical response. This approach will hone your intuition and serve to refine your clinical thought processes. Remember, practice doesn’t make perfect, perfect practice makes perfect.
Basics of sweep gas flow titration
Recall that the oxygenator membrane is semi-permeable, allowing for O 2 and CO 2 to diffuse down their respective concentration gradients and that while both molecules are able to move across the membrane, the diffusibility of CO 2 is six times greater than the diffusibility of O 2 ( Fig. 18.1 ).

This higher diffusibility of CO 2 means that the rate of gas flow directly correlates with how fast CO 2 is cleared. The higher the rate of gas flow, the faster CO 2 is removed from the blood.
This concept underlies the convention provided that PaCO 2 is primarily affected by adjustments to flow rate of sweep gas , while PaO 2 of the blood leaving the oxygenator is primarily affected by adjustments to the FiO 2 of the sweep gas flow ( Fig. 18.2 ).

For the most part, adjustments of 1 L or greater should be made with the middle knob (increments of 0.5 L) while adjustments to sweep of <1 L should be made with the knob on the left (increments of 100mL), to allow for more precise titration. These two knobs will be additive, so that if the middle knob is set to 4 L/min and the left knob is set to 500 mL/min, the patient will be receiving 4.5 L/min of sweep gas flow.
How much does an adjustment in sweep gas flow affect PaCO 2 of arterial blood? The answer lies in the efficiency of the membrane oxygenator, the presence of recirculation, minute ventilation and dead space of the native lungs, and the CO 2 gradient, which is a function of PaCO 2 entering into the membrane oxygenator via the venous blood.
As a general rule of thumb, an increase in sweep gas flow by 1 L/min can be expected to decrease PaCO 2 by 5–10 mmHg.
The presence of the aforementioned mitigating factors requires that adjustments to sweep gas flow are put into the correct clinical context. Whenever possible, confirm the result of changes in sweep by monitoring the clinical response of the patient (dyspnea, tachypnea, apnea, encephalopathy, etc.) as well as the patient arterial blood gas when clinically appropriate.
Placing sweep gas flow into the clinical phase of ECMO support
“Easy enough, when CO 2 is high, go up on sweep and when CO 2 is low go down on sweep, right?” While this is sometimes the case, there is often more subtlety to the titration of sweep gas flow.
The first consideration is what phase of ECMO support the patient is in. While the clinical characteristics of an ECMO run can vary, with setbacks and improvements throughout, we can expect an overall pattern involving three distinct phases: stabilization, maintenance, and weaning. The way we adjust and titrate sweep gas flow will differ significantly depending on what phase we are in. Let’s use the graph in Fig. 18.3 to illustrate.

Stabilization: Stabilization is the period where we are trying to manage and mitigate end organ damage. We are trying to prevent the vicious cycle of cardiac and respiratory failure that could lead to multiorgan failure, with progressive and sequential shutdown of peripheral tissue beds.
During this period, sweep gas flow titration tends to be much more aggressive, with an emphasis on correcting acidosis as well as CO 2 in order to optimize right ventricular afterload, cerebral perfusion, as well as perfusion to end organ tissue beds.
When initiating ECMO, the common convention is to initiate sweep at a 1:1 rate with blood flow and adjust thereafter based on clinical/laboratory parameters. As an example, if you initiate ECMO and the blood flow is set to 3 L/min, sweep gas can be set to 3 L/min with the plan to check arterial blood gases 20–30 minutes after initiating ECMO.
Maintenance: This is the period where stabilization has occurred but the patient still needs ECMO support. The focus of the overall management shifts from mitigating further decompensation to advancing rehabilitation, optimizing nutrition, weaning sedation, and preventing and managing complications.
The length of this period may range from days to weeks depending on the level of support and the overall course of disease.
Sweep gas flow targets in this phase are aimed towards maintaining lung-protective/ultra–lung-protective ventilation, preventing encephalopathy, and patient comfort by titrating to prevent dyspnea/apnea.
When it comes to sweep gas in this phase, there is a rationale/advantage for parsimony. If the patient is not clinically impacted, uncomfortable, or encephalopathic, and if lung-protective ventilation is maintained, maintaining less sweep allows for the ability to increase when needed and allows for engagement of the lungs in CO 2 clearance. Similar to our discussion with blood flow titration, just because you can flow at a higher sweep does not mean you should flow higher.
Weaning: This is often the most gratifying phase. As the heart/lungs improve, dead space decreases, and V/Q mismatch improves. Additionally, fluid is mobilized from the pulmonary interstitium into the intravascular space, with improved pulmonary compliance, better minute ventilation, and more CO 2 clearance from the native lungs.
This is the phase where sweep can be weaned more aggressively, allowing the lungs to take on more of the load of CO 2 clearance. Sweep can be downtitrated if patient is in the weaning phase, even if the PaCO 2 is normal or even modestly elevated.
Confirm that you are truly in the weaning phase by assessing as many clinical variables as you can. Some questions to ask include:
- •
Is the compliance on the ventilator improving?
- •
Is the chest X-ray clear/improved?
- •
Is there evidence of heart/lung recovery in terms of oxygenation (improved PaO 2 )?
- •
Is there evidence of mobilization of fluid with increased urine output and net negative fluid balance despite minimal or stable diuretics?
- •
Has blood flow been decreased with minimal impact on clinical status?
As more and more of these scenarios become true, the assumption that the heart/lungs are recovering becomes an increasingly reasonable proposition.
However, note that this can only be done if the patient is truly improved and the lungs are ready to take on the burden of increased CO 2 clearance. If not, this can lead to injury to the lungs, especially if weaning requires a significant escalation in ventilator settings. Patience is paramount – the heart/lungs will take over when they are ready.
Impact of sweep gas flow on CO 2 buffering
CO 2 dissolves in water to form carbonic acid, which dissociates to bicarbonate/hydrogen ion based on the following equilibrium: