CHAPTER 65
Rib Fracture and Costochondral Separation
(Broken Rib)
Presentation
A patient with an isolated rib fracture or a minor costochondral separation usually has recently fallen, injuring the side of the chest; been struck by a blunt object; coughed violently; or leaned over a rigid edge. The initial chest pain may subside, but over the next few hours or days the pain increases with movement, interferes with sleep and activity, and becomes severe when the patient coughs or breathes deeply. The patient is often worried about having a broken rib and may have a sensation of bony crepitus or abnormal rib movement. Breath sounds bilaterally should be normal, unless there is substantial splinting or a pneumothorax or hemothorax is present. There is point tenderness over the site of the injury, and occasionally bony crepitus can be felt.
What To Do:
 Examine the patient for possible associated injuries, and palpate the abdomen for any signs of a splenic or hepatic injury. What appear to be insignificant mechanisms of injury, such as falling over a chair, hitting the edge of a table, or colliding into a strong ocean wave all have resulted in splenic rupture. Maintain a high index of suspicion of severe underlying injuries. Consider intra-abdominal injuries in all patients with lower rib fractures and mediastinal injury in those with fractures of the first three ribs. Keep a low threshold for ordering CT scans, especially in the patient with altered mental status or other distracting injuries.
Examine the patient for possible associated injuries, and palpate the abdomen for any signs of a splenic or hepatic injury. What appear to be insignificant mechanisms of injury, such as falling over a chair, hitting the edge of a table, or colliding into a strong ocean wave all have resulted in splenic rupture. Maintain a high index of suspicion of severe underlying injuries. Consider intra-abdominal injuries in all patients with lower rib fractures and mediastinal injury in those with fractures of the first three ribs. Keep a low threshold for ordering CT scans, especially in the patient with altered mental status or other distracting injuries.

 When there is a history of minor trauma and you do not suspect an intra-abdominal injury, check for rib pain and clinical evidence of fracture by applying indirect stress to the suspected fracture site. Compress the rib anteroposteriorly if a fracture is suspected at a lateral location. Compress the rib medially if a posterior or anterior fracture is suspected (Figure 65-1). Pain occurring at the suspected fracture site during application of indirect stress is clinical evidence of a fracture or separation and should be documented on the chart as a “clinical rib fx.” If there is pain with deep inspiration or cough and point tenderness at any position along the rib contours that reproduces this pain, a diagnosis of a clinical rib fracture can also be made. If subcutaneous emphysema is appreciated on examination, the patient is at risk for delayed pneumothorax and should be admitted for observation.
When there is a history of minor trauma and you do not suspect an intra-abdominal injury, check for rib pain and clinical evidence of fracture by applying indirect stress to the suspected fracture site. Compress the rib anteroposteriorly if a fracture is suspected at a lateral location. Compress the rib medially if a posterior or anterior fracture is suspected (Figure 65-1). Pain occurring at the suspected fracture site during application of indirect stress is clinical evidence of a fracture or separation and should be documented on the chart as a “clinical rib fx.” If there is pain with deep inspiration or cough and point tenderness at any position along the rib contours that reproduces this pain, a diagnosis of a clinical rib fracture can also be made. If subcutaneous emphysema is appreciated on examination, the patient is at risk for delayed pneumothorax and should be admitted for observation.
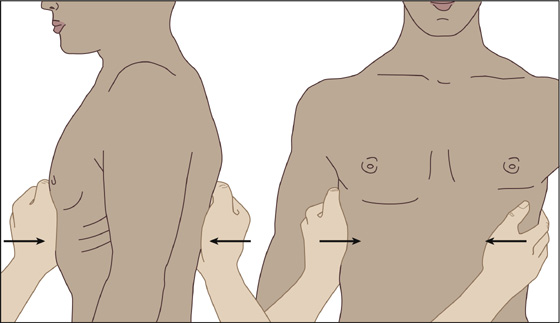
Figure 65-1 Indirect stress test with anteroposterior compression to reveal a lateral rib fracture and lateral-medial compression to reveal an anterior or posterior fracture.
 Obtain any history of chronic pulmonary problems or heavy smoking.
Obtain any history of chronic pulmonary problems or heavy smoking.
 Send the patient for posteroanterior and lateral chest radiographs to rule out a pneumothorax, hemothorax, and pulmonary contusion. Additional oblique rib films for radiologic documentation of a fracture are generally not recommended and rarely add clinical or therapeutic benefit, especially with anterior cartilage injuries. These films may be indicated to document the extent of injury when there is a suspicion of multiple rib fractures, especially in the elderly patient.
Send the patient for posteroanterior and lateral chest radiographs to rule out a pneumothorax, hemothorax, and pulmonary contusion. Additional oblique rib films for radiologic documentation of a fracture are generally not recommended and rarely add clinical or therapeutic benefit, especially with anterior cartilage injuries. These films may be indicated to document the extent of injury when there is a suspicion of multiple rib fractures, especially in the elderly patient.
 Elderly patients with multiple rib fractures have an increased incidence of pneumonia and overall increased mortality and usually require hospital admission with aggressive analgesic management and respiratory care.
Elderly patients with multiple rib fractures have an increased incidence of pneumonia and overall increased mortality and usually require hospital admission with aggressive analgesic management and respiratory care.
 If there is no suspicion of a more serious underlying injury, and there is clinical or radiologic evidence of a rib fracture or chondral separation, provide as potent an oral analgesic as needed to control pain. Ibuprofen, naproxen, acetaminophen plus hydrocodone, or acetaminophen plus oxycodone are examples of nonsteroidal anti-inflammatory drugs (NSAIDs) and narcotic preparations that are often most effective when used in combination.
If there is no suspicion of a more serious underlying injury, and there is clinical or radiologic evidence of a rib fracture or chondral separation, provide as potent an oral analgesic as needed to control pain. Ibuprofen, naproxen, acetaminophen plus hydrocodone, or acetaminophen plus oxycodone are examples of nonsteroidal anti-inflammatory drugs (NSAIDs) and narcotic preparations that are often most effective when used in combination.
 If available, and if the patient is young and healthy, you can place a rib belt on the patient to see if this provides comfort. If there is significant pain relief, you can instruct the patient regarding the intermittent use of this elastic and Velcro belt. Place the bottom of the belt at the inferior tip of the xiphoid process, tightening it around the chest enough to obtain maximum pain relief. The rib belt may be worn almost continuously for the first 1 to 4 days, but it should be removed as comfort allows thereafter (Figure 65-2).
If available, and if the patient is young and healthy, you can place a rib belt on the patient to see if this provides comfort. If there is significant pain relief, you can instruct the patient regarding the intermittent use of this elastic and Velcro belt. Place the bottom of the belt at the inferior tip of the xiphoid process, tightening it around the chest enough to obtain maximum pain relief. The rib belt may be worn almost continuously for the first 1 to 4 days, but it should be removed as comfort allows thereafter (Figure 65-2).
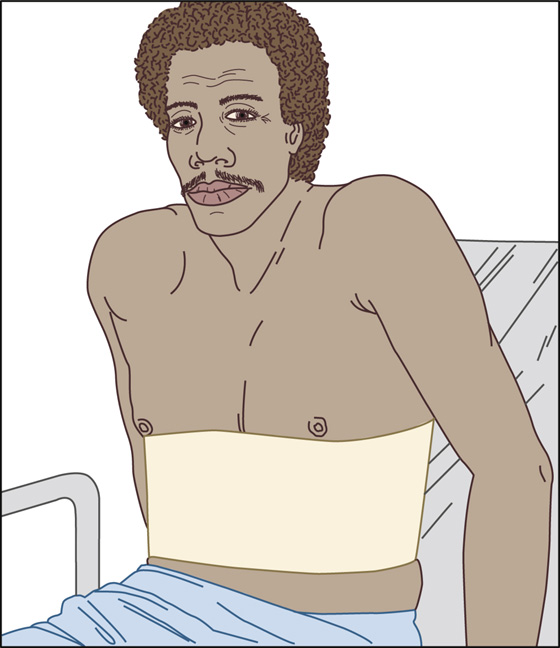
Figure 65-2 Proper placement of elastic and Velcro rib belt.
 Instruct the patient regarding the importance of deep breathing and coughing (without the rib belt but using a pillow splint) to help prevent pneumonia. Tell him to take enough pain medicine to allow coughing and deep breathing. When available, provide incentive spirometry.
Instruct the patient regarding the importance of deep breathing and coughing (without the rib belt but using a pillow splint) to help prevent pneumonia. Tell him to take enough pain medicine to allow coughing and deep breathing. When available, provide incentive spirometry.
 Provide the patient with appropriate documentation for missing work, and refer him for follow-up care in 48 hours. Tell him to expect gradually decreasing discomfort for about 2 to 4 weeks, but prepare him for an extended period of disability (it will take several weeks to heal and become pain free). Forbid strenuous activity for approximately 8 weeks. One study showed that patients with isolated rib fractures returned to work or their usual activities at a mean of 51 days (±39 days).
Provide the patient with appropriate documentation for missing work, and refer him for follow-up care in 48 hours. Tell him to expect gradually decreasing discomfort for about 2 to 4 weeks, but prepare him for an extended period of disability (it will take several weeks to heal and become pain free). Forbid strenuous activity for approximately 8 weeks. One study showed that patients with isolated rib fractures returned to work or their usual activities at a mean of 51 days (±39 days).
 Severe worsening of chest pain, shortness of breath, fever, or purulent sputum may signal pulmonary complications and should prompt a return visit. A greater incidence of complications can be expected in patients with displaced rib fractures.
Severe worsening of chest pain, shortness of breath, fever, or purulent sputum may signal pulmonary complications and should prompt a return visit. A greater incidence of complications can be expected in patients with displaced rib fractures.
 When there is no clinical or radiologic evidence of a fracture, treat the pain as any other contusion would be treated, using an appropriate analgesic.
When there is no clinical or radiologic evidence of a fracture, treat the pain as any other contusion would be treated, using an appropriate analgesic.
What Not To Do:
 Do not confuse simple rib fractures with massive blunt trauma to the chest. The evaluation and management are quite different.
Do not confuse simple rib fractures with massive blunt trauma to the chest. The evaluation and management are quite different.
 Do not overlook child or elder abuse. Rib fractures are uncommon in younger children and are found in 5% to 27% of documented cases of child abuse. Child abuse should be considered in the absence of a plausible history of trauma or conditions of bony fragility, such as osteogenesis imperfecta or rickets.
Do not overlook child or elder abuse. Rib fractures are uncommon in younger children and are found in 5% to 27% of documented cases of child abuse. Child abuse should be considered in the absence of a plausible history of trauma or conditions of bony fragility, such as osteogenesis imperfecta or rickets.
 Do not tape ribs or use continuous strapping. This will lead to hypoventilation and an atelectatic lung that is prone to pneumonia.
Do not tape ribs or use continuous strapping. This will lead to hypoventilation and an atelectatic lung that is prone to pneumonia.
 Do not assume that there is no fracture just because the radiographs are normal. Rib fractures are often not apparent on radiographs, especially when they occur in the cartilaginous portion of the rib. The patient deserves the disability period and analgesics commensurate with the real injury.
Do not assume that there is no fracture just because the radiographs are normal. Rib fractures are often not apparent on radiographs, especially when they occur in the cartilaginous portion of the rib. The patient deserves the disability period and analgesics commensurate with the real injury.
Discussion
Rib fracture pain can be significant, originates at the site of the fractured bone and injured muscle, and is usually reported by patients to be exacerbated by any movement of the chest wall (e.g., with respiration and most certainly with deep breathing and coughing). Although most commonly secondary to trauma, rib fractures may also occur because of repetitive stressors, such as that experienced with coughing or in athletes such as golfers and rowers.
Most isolated fractures and separations cause minimal morbidity or mortality and are treated with immobilization, but ribs are a special problem because patients have to continue breathing. Pain management is crucial. Patients with pain often splint and hypoventilate and thus are predisposed to pneumonia. Outpatient management of isolated rib fractures with oral pain medication is generally adequate.
In the presence of severe pain or multiple rib fractures, consider the use of an intercostal nerve block or injection of the fracture hematoma with 0.5% bupivacaine (Marcaine). Because of the risk for pneumothorax or hemothorax, in most cases, this procedure should be reserved for secondary management when initial treatment has proven inadequate.
Although rib belts are no longer commonly used and their use is even discouraged, they can sometimes provide significant pain relief for young, active patients who are at low risk for pulmonary complications. If used, it may be worn almost continuously for the first 1 to 4 days, but it should be removed as comfort allows thereafter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


