CHAPTER 34
Otitis Externa (Swimmer’s Ear), Acute
Presentation
In acute otitis externa (AOE), the patient complains of ear pain, which is always uncomfortable and sometimes unbearable, often accompanied by drainage and a blocked sensation, decreased hearing, and sometimes by fever. When the condition is mild or chronic, there may be itching rather than pain. Pulling on the auricle or pushing on the tragus of the ear classically causes increased pain (Figure 34-1). The tissue lining of the canal may be swollen, and, in severe cases, the swelling can extend into the soft tissue surrounding the ear. Tender erythematous swelling or an underlying furuncle may be present, and it may be pointing or draining.
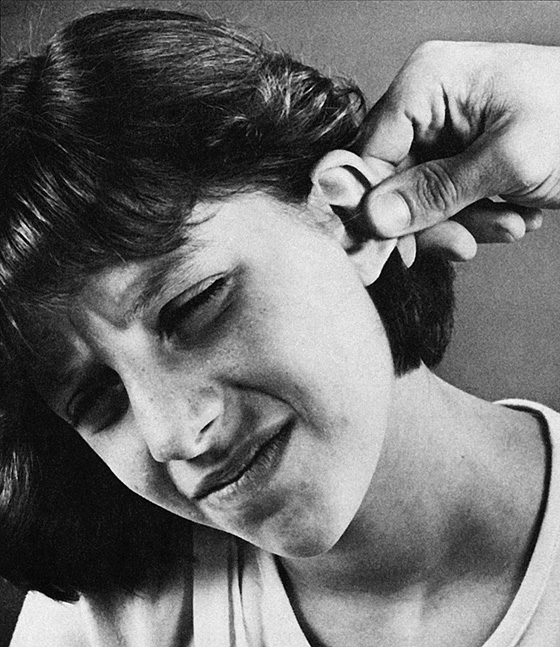
Figure 34-1 Pulling on the ear causes increased pain.
The canal may be erythematous and dry, or it may be covered with fuzzy cotton-like grayish or black fungal plaques (wet newspaper appearance). Most often, the canal lining is moist and covered with purulent drainage and debris, and cerumen is characteristically absent. The canal may be so swollen that it is difficult or impossible to view the tympanic membrane (TM), which, when visible, often looks dull.
A pruritic vesiculopapular eruption in the canal is most consistent with an allergic reaction to a topical agent (often neomycin) (see Chapter 160).
What To Do:
 Determine if the patient has had tympanostomy tubes or a history of chronic suppurative otitis media with recurrent ear drainage; if so, he will probably have an open TM.
Determine if the patient has had tympanostomy tubes or a history of chronic suppurative otitis media with recurrent ear drainage; if so, he will probably have an open TM.
 Meticulous and repeated clearing of the canal is the cornerstone of treatment. Irrigation can be very effective in cleaning out the canal, using a 1:1 dilution of 3% hydrogen peroxide (if the TM is intact). Other cleaning methods include suction, cotton swabs, and ear curettes.
Meticulous and repeated clearing of the canal is the cornerstone of treatment. Irrigation can be very effective in cleaning out the canal, using a 1:1 dilution of 3% hydrogen peroxide (if the TM is intact). Other cleaning methods include suction, cotton swabs, and ear curettes.
 Inspect the ear for the presence of a foreign body.
Inspect the ear for the presence of a foreign body.
 Incise and drain any furuncle that is pointing or fluctuant.
Incise and drain any furuncle that is pointing or fluctuant.
 If the ear canal is too narrow to allow medication to flow freely, insert a wick. The best wick is the Pope ear wick (Merocel Corporation, Mystic, Conn.), which is about 1 × 10 mm of compressed cellulose; it is thin enough to slip into an occluded canal but expands when wet. If this wick is not available, try using alligator forceps to insert a 1-cm strip of ¼-inch plain gauze or a twisted wisp of cotton that may be obtained from a cotton ball or the end of a cotton-tipped applicator. (This method is more painful.) Advance the wick cautiously to avoid damaging the middle-ear structures or puncturing the TM. After the wick is inserted, water must be kept out of the ear, and the patient must be instructed to use soft wax earplugs while showering. Wicks may be replaced every 1 to 3 days if the symptoms persist.
If the ear canal is too narrow to allow medication to flow freely, insert a wick. The best wick is the Pope ear wick (Merocel Corporation, Mystic, Conn.), which is about 1 × 10 mm of compressed cellulose; it is thin enough to slip into an occluded canal but expands when wet. If this wick is not available, try using alligator forceps to insert a 1-cm strip of ¼-inch plain gauze or a twisted wisp of cotton that may be obtained from a cotton ball or the end of a cotton-tipped applicator. (This method is more painful.) Advance the wick cautiously to avoid damaging the middle-ear structures or puncturing the TM. After the wick is inserted, water must be kept out of the ear, and the patient must be instructed to use soft wax earplugs while showering. Wicks may be replaced every 1 to 3 days if the symptoms persist.
 Studies have shown no difference in cure rate between topical antibiotics, topical antiseptics and topical antibiotic/steroid preparations, but that these agents are significantly superior to placebo.
Studies have shown no difference in cure rate between topical antibiotics, topical antiseptics and topical antibiotic/steroid preparations, but that these agents are significantly superior to placebo.
 Acidifying solutions, such as acetic acid, work by lowering canal pH, thus inhibiting fungal and bacterial growth. The addition of a steroid to the antimicrobial or acidifying solution has been shown to decrease time to symptom relief. A typical acidifying solution is 2% acetic acid. (Add 2 parts of 5% acetic acid [or household vinegar] to 3 parts water and you will render 2% acetic acid.) Pseudomonas aeruginosa and Staphylococcus are the most common bacteria responsible for AOE.
Acidifying solutions, such as acetic acid, work by lowering canal pH, thus inhibiting fungal and bacterial growth. The addition of a steroid to the antimicrobial or acidifying solution has been shown to decrease time to symptom relief. A typical acidifying solution is 2% acetic acid. (Add 2 parts of 5% acetic acid [or household vinegar] to 3 parts water and you will render 2% acetic acid.) Pseudomonas aeruginosa and Staphylococcus are the most common bacteria responsible for AOE.
 There are several antibiotic choices, but ciprofloxacin and ofloxacin have the advantage of good bacterial coverage, bid dosing, and ability to use if the TM is perforated. Suggestions are ciprofloxacin-hydrocortisone (Cipro HC Otic) otic suspension, 10 mL, 3 drops in ear(s) bid × 7 days, or ofloxacin (Floxin Otic), 10 mL, 0.3%, 5 drops in ear(s) bid × 7 days. If the TM is intact, other choices are gentamycin (Garamycin) or tobramycin (Tobrex) ophthalmic solution 0.3%, 5 mL, 4 to 6 drops in ear(s) qid × 7 days.
There are several antibiotic choices, but ciprofloxacin and ofloxacin have the advantage of good bacterial coverage, bid dosing, and ability to use if the TM is perforated. Suggestions are ciprofloxacin-hydrocortisone (Cipro HC Otic) otic suspension, 10 mL, 3 drops in ear(s) bid × 7 days, or ofloxacin (Floxin Otic), 10 mL, 0.3%, 5 drops in ear(s) bid × 7 days. If the TM is intact, other choices are gentamycin (Garamycin) or tobramycin (Tobrex) ophthalmic solution 0.3%, 5 mL, 4 to 6 drops in ear(s) qid × 7 days.
 Fungal infections cause about 10% of AOE. Patients usually complain more of itching than pain, and edema of the canal is often milder than in bacterial infection. Fungal filaments can sometimes be seen, and Candida typically reveals sebaceous-like material in the canal. Topical antifungals, such as acetic acid and aluminum acetate (Domeboro Otic), 60 mL, 4 to 6 drops in ear(s) q2-3h × 7 days; acetic acid (VoSol Otic) 15%, 30 mL, 5 drops in ear(s) tid to qid (VoSol HC Otic adds hydrocortisone 1% [only generic is available]); or clotrimazole (Lotrimin) 10 mL, 1% solution, 4 to 6 drops in ear(s) bid × 7 days, may be prescribed. Acetic acid preparations should not be used if an open TM is known or suspected to be present because of theoretical ototoxicity.
Fungal infections cause about 10% of AOE. Patients usually complain more of itching than pain, and edema of the canal is often milder than in bacterial infection. Fungal filaments can sometimes be seen, and Candida typically reveals sebaceous-like material in the canal. Topical antifungals, such as acetic acid and aluminum acetate (Domeboro Otic), 60 mL, 4 to 6 drops in ear(s) q2-3h × 7 days; acetic acid (VoSol Otic) 15%, 30 mL, 5 drops in ear(s) tid to qid (VoSol HC Otic adds hydrocortisone 1% [only generic is available]); or clotrimazole (Lotrimin) 10 mL, 1% solution, 4 to 6 drops in ear(s) bid × 7 days, may be prescribed. Acetic acid preparations should not be used if an open TM is known or suspected to be present because of theoretical ototoxicity.
 For moderate to severe pain and soft tissue swelling or other signs of cellulitis, prescribe an appropriate analgesic. Systemic antibiotics are indicated in patients with diabetes mellitus, immunodeficiency, history of radiation to the ear, or when infection has spread beyond the external ear canal, or if the canal cannot be adequately cleared to allow the topical agent to work. Systemic antibiotics include levofloxacin (Levaquin), 500 mg qd × 10 days, or ciprofloxacin (Cipro) 500 mg bid × 10 days.
For moderate to severe pain and soft tissue swelling or other signs of cellulitis, prescribe an appropriate analgesic. Systemic antibiotics are indicated in patients with diabetes mellitus, immunodeficiency, history of radiation to the ear, or when infection has spread beyond the external ear canal, or if the canal cannot be adequately cleared to allow the topical agent to work. Systemic antibiotics include levofloxacin (Levaquin), 500 mg qd × 10 days, or ciprofloxacin (Cipro) 500 mg bid × 10 days.
 Provide follow-up in 2 to 3 days to remove a wick and any remaining debris from the ear canal.
Provide follow-up in 2 to 3 days to remove a wick and any remaining debris from the ear canal.
 When administering ear drops without a wick, instruct the patient to lie on her side for 20 minutes after instilling, to maximize medication exposure.
When administering ear drops without a wick, instruct the patient to lie on her side for 20 minutes after instilling, to maximize medication exposure.
What Not To Do:
 Do not routinely culture ear drainage. This should be reserved for severe cases or where there is persistent or refractory infection.
Do not routinely culture ear drainage. This should be reserved for severe cases or where there is persistent or refractory infection.
 Do not use oral antibiotics to treat simple otitis externa without evidence of cellulitis or concurrent otitis media.
Do not use oral antibiotics to treat simple otitis externa without evidence of cellulitis or concurrent otitis media.
 Do not use topical antibiotics for prophylaxis. Long-term use of any topical antibiotics can lead to a fungal superinfection.
Do not use topical antibiotics for prophylaxis. Long-term use of any topical antibiotics can lead to a fungal superinfection.
 Do not instill medication without first cleansing the ear canal, unless restricted because of pain and/or swelling.
Do not instill medication without first cleansing the ear canal, unless restricted because of pain and/or swelling.
 Do not expect medicine to enter a canal that is swollen shut without using a wick.
Do not expect medicine to enter a canal that is swollen shut without using a wick.
 Do not use eardrops containing neomycin, which sometimes causes severe allergic contact dermatitis.
Do not use eardrops containing neomycin, which sometimes causes severe allergic contact dermatitis.
 Do not miss the case of malignant (necrotizing) external otitis in the elderly diabetic patient who presents with exquisitely painful otorrhea. These patients require otolaryngologic consultation, special diagnostic evaluation, and prolonged administration of an oral quinolone.
Do not miss the case of malignant (necrotizing) external otitis in the elderly diabetic patient who presents with exquisitely painful otorrhea. These patients require otolaryngologic consultation, special diagnostic evaluation, and prolonged administration of an oral quinolone.
Discussion
Acute otitis externa has a seasonal occurrence, being more frequently encountered in the summer months, when the climate and contaminated swimming water will most likely precipitate a fungal or Pseudomonas aeruginosa bacterial infection. P. aeruginosa is the most common bacterium involved in this infection, with Staphylococcus species being the next most common pathogen. Fungi are only responsible for approximately 2% of cases but may well be more prominent in cases of persistent or chronic infection. Various dermatoses, diabetes, aggressive ear cleaning with cotton-tipped swabs, previous external ear infections, and furunculosis also predispose patients to developing otitis externa.
The healthy ear canal is coated with cerumen and sloughed epithelium. Cerumen is water repellent and acidic and contains a number of antimicrobial substances. Repeated washing or cleaning can remove this defensive coating. Moisture retained in the ear canal is readily absorbed by the stratum corneum. The skin becomes macerated and edematous, and the accumulation of debris may block gland ducts, preventing further production of the protective cerumen. Finally, endogenous or exogenous organisms invade the damaged canal epithelium and cause the infection.
In most cases of uncomplicated acute otitis externa, topical antibiotics are the first-line treatment choice. There is no evidence that systemic antibiotics alone or combined with topical preparations improve treatment outcome compared with topical antibiotics alone, and they may contribute to the development of bacterial resistance. When a perforation exists or a patent tympanostomy tube is present, quinolone drops offer superior safety and efficacy. It should be realized, however, that the risk for ototoxicity is negligible when using aminoglycoside combination drops or acetic acid drops when the TM is intact, and that these preparations are consistently effective and less expensive first-line treatments. Clearly, systemic antibiotics are indicated to treat the more serious manifestations of the disease, such as periauricular cellulitis or necrotizing otitis externa.
Malignant or necrotizing external otitis is a potentially life-threatening condition that occurs primarily in elderly diabetic patients and immunocompromised individuals. P. aeruginosa is isolated from the aural drainage in more than 90% of cases. The pathophysiology is incompletely understood, although irrigation for cerumen impaction has been reported as a potential iatrogenic factor.
The typical patient presents with severe headache or ear pain, swelling, and drainage. Granulation tissue on the floor of the ear canal may be present. The TM is almost always intact. Disease progression is associated with osteomyelitis of the skull base and temporomandibular joint. Cranial nerve palsies generally indicate advancing infection. Paralysis of the facial nerve is most common. Patients are usually afebrile with normal white blood cell (WBC) and differential counts. The erythrocyte sedimentation rate (ESR) is usually markedly increased. CT scans are ideal to assess for bone erosion. In a prospective study, presence of bone erosion and soft tissue abnormalities in the infratemporal fossa were most helpful in making the diagnosis of malignant external otitis. There is no role for topical antibiotics, even quinolones, in the treatment of this disease. Instillation of antipseudomonal topical agents only increases the difficulty of isolating the pathogenic organism from the ear canal. Systemic antipseudomonal antibiotics are the primary therapy for malignant external otitis. The availability of oral agents has eliminated the need for hospitalization in all but the most recalcitrant cases. Ciprofloxacin (Cipro), 750 mg orally bid, seems to be the antibiotic of choice. Despite the rapid relief of symptoms (pain and otorrhea), prolonged treatment for 6 to 8 weeks is still recommended, as indicated for osteomyelitis. Early consultation should be obtained if there is any suspicion of this condition in a susceptible patient with a draining ear.
The ear is innervated by the fifth, seventh, ninth, and tenth cranial nerves and the second and third cervical nerves. Because of this rich nerve supply, the skin is extremely sensitive. Otalgia may arise directly from the seventh cranial nerve (geniculate ganglion), ninth cranial nerve (tympanic branch), external ear, mastoid air cells, mouth, teeth, or esophagus. Ear pain can result from sinusitis, trigeminal neuralgia, and temporomandibular joint dysfunction or may be referred from disorders of the pharynx and larynx. A mild pain referred to the ear may be felt as itching, may cause the patient to scratch the ear canal, and may present as external otitis.
It is important to consider the possibility of malignancy in the evaluation of a patient with otalgia and apparently refractory otitis externa. When the source of ear pain is not readily apparent, the patient should be referred for a more complete otolaryngologic investigation.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


