background and perspective from the US
The three cases
Please refer to the previous chapter’s cases for discussion.
Opium addiction as a social problem
Although opium derivatives have been used since antiquity for medicinal and recreational purposes, recognition of opioid addiction as a significant social problem emerged only relatively recently. The opium eaters of the eighteenth and nineteenth centuries consumed fairly low doses of active drug. Intoxication and addiction certainly existed, but the lack of widespread availability prevented broad societal ramifications. Nonetheless, a stigma was attached to opium consumption by a largely religious society that valued suffering as a moral good. The Quakers, for example, likened the soul to a physical entity; intoxicating substances impaired self-restraint, leading to lapses in moral judgment and consequent damage to the soul. Despite these views, few restrictions on opium existed.
With the emergence of purified morphine and later heroin, the deleterious effects of opioids on individuals and society came into focus. In the US, the number of narcotic addicts exploded, crime rose, and worker productivity declined. Legislation soon followed. The Harrison Act of 1914 restricted opioid and cocaine distribution to registered physicians and pharmacies. By the 1920s, authorities jailed physicians for distributing opioids outside their professional “course of conduct,” thus setting a precedent that would affect opioid prescribing for decades. Britain soon followed with its own legislation, the Dangerous Drugs Act, in 1920.
Regulatory influence
In the US, after Webb versus the United States1 and provisions of the 1914 Harrison Narcotic Drug Act made it illegal for physicians to prescribe opioids for the treatment of opioid addiction, opioid treatment of pain practically ceased. Not knowing which of their patients might be addicted, doctors in the US were intimidated lest they lose their medical license, or worse still, suffer criminal prosecution. The laws in other Western countries were less constraining. In the UK, guided by the Rolleston Committee (1924–1965), physicians were allowed to give their addicted patients diamorphine (heroin), syringes, and needles. At the time, heroin proliferation was less of a problem in the UK than in the US: in 1958 there were only 62 known heroin users in the UK, a number that would soon increase several-fold. In The (London) Times in 1955 it was argued:
In a description of the London drug scene in the 1960s, the preacher Kenneth Leech wrote:
‘To cut off the supply by prescription would be easy; it has been done in the United States where doctors are not allowed to prescribe for addicts, with the result that the provision of drugs has become a flourishing industry and drug addiction increases there yearly.’4
The differences between the US and other Western countries persisted into the late 1960s when US President Richard Nixon’s “War on Drugs” led to even stricter regulations. The effect on the medical use of opioids in the US was disastrous. By the second half of the twentieth century, both addiction and pain were undertreated, with baleful consequences. When the iniquities of undertreatment were recognized, opioid advocacy was born. In the US, addiction advocacy brought about the re-establishment of opioid (methadone) treatment for addiction in 1974 (Narcotic Addict Treatment Act); pain advocacy during the 1970s and 1980s brought about the re-establishment of opioids for the treatment of acute and cancer pain, principles that were later extended to chronic pain.
Prevalence of prescription opioid abuse
Historically, under-treatment of pain as a consequence of draconian anti-drug laws occurred mainly in the US. The swing of the pendulum towards over-use, or at least careless use, of opioids for pain seems also a uniquely American problem,5 reflected in alarming statistics that demonstrate precipitous increases in prescription opioid abuse over the past decade, to the extent that prescription opioid abuse is now more prevalent in the US than is illicit heroin abuse.6 (Figure 26.1) Successful marketing of “designer” opioids increased prescribing of opioids for chronic pain.7 Increased prescribing for pain resulted in increased opioid analgesics in homes, pharmacies, and on the streets, and has likely contributed to the disturbing increases in prescription drug abuse and related deaths seen in the US.8 Surveys such as the National Household Survey do not exist in the UK, and it may be that, without an effective early warning system, the extent of the problem of prescription opioid abuse is unknown in UK.9 Whatever the benefits of the UK’s relatively forgiving approach to controlling addiction in terms of not having inhibited opioid prescribing for pain to the same extent as in the US, UK policies seem to be failing to control problematic illicit drug use when compared to other European countries. The UK now has the worst illicit drug problem in Europe, a situation that is bound to impact UK general practitioners at the intersection of pain and addiction. Effective confinement of prescription opioid use to medical use, as appears to have been achieved in the UK, seems ideal, yet the balance between prescription and illicit opioid abuse will always be precarious.
Enactment of laws and their effect on opioid prescribing for pain
In the US, the Controlled Substances Act of 1970 unified many previous laws under a single framework regulating the manufacture, distribution, prescription, and dispensing of opioids and other substances with abuse potential. Controlled substances were assigned to one of five schedules based on their medical utility and abuse potential. The Controlled Substance Act defines neither legitimate medical purpose nor standards of professional practice: this falls to the state medical boards, professional societies, the Department of Justice, or even lay juries in criminal trials. Criminal charges against physicians generally arise only when both bad practice and bad intention by the practitioner are established.
Because of legal constraints placed on opioid prescribing in the US, gross negligence (bad practice) may lead to criminal prosecution even when there is good intention. For example, a physician is more likely to be accused of involuntary manslaughter if the drug chosen for overdose by a suicidal patient is an opioid rather than a noncontrolled drug such as a tricyclic antidepressant. In People v Schade, a physician was convicted of involuntary manslaughter when a patient with known addiction and suicidal ideation killed himself with an opioid that had been prescribed within days of a previous suicide attempt. The jury deemed this to be reckless facilitation of a suicide. Had the medication not been a controlled substance, the physician more likely would
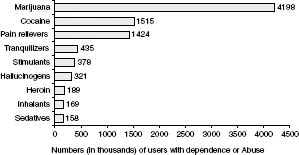
Figure 26.1. Dependence or Abuse of Specific Illicit Drugs among Persons Aged 12 or Older: 2003
have faced malpractice (a civil action not subject to incarceration), rather than criminal charges.10
The perception of risk of even being investigated, let alone being tried and convicted on criminal charges, has deterred many physicians from aggressively treating pain with controlled substances. In the US there is a risk also of being charged with undertreatment of pain. In 2001 a California physician was convicted of elder abuse for underprescribing pain medications in a malpractice suit. The jury awarded the family $1.5 million.11 Cases such as these have raised significant societal debate on the role of the courts in dictating what constitutes a “legitimate medical purpose,” a role historically the purview of state medical boards and professional societies. Contradictory legal precedent places physicians in a quandary: prescribe liberally and risk possible criminal investigation or prescribe sparingly and risk civil proceedings for the undertreatment of pain. The war on drugs collides with another American phenomenon, patient advocacy for the right to pain control. Physicians are left caught in the middle.
Because UK drug regulations are less restrictive than those in the US, criminal prosecution of physicians on charges related to opioids were virtually unheard of until the notorious case of Harold Shipman in 1998. Harold Shipman was a general practitioner who was tried and convicted of the murders of 15 elderly patients. He had administered diamorphine (a legal drug in the UK for clinical use). After his trial, a special inquiry (the Shipman Inquiry) found evidence to suggest that he had, in fact, killed as many as 250 people. The press coverage of the case was such that Harold Shipman’s activities became well known in the UK. Unlike the US, where criminal prosecution of physicians had occurred relatively frequently with an insidious effect on opioid prescribing for pain, the Shipman case had an immediate and profound effect on opioid prescribing in the UK. The Shipman Inquiry was damning in its criticism of the General Medical Council (the body that accredits British doctors) saying that the body had protected doctors at the expense of protecting patients.12 The inquiry suggested two ways in which risk might be reduced, which had been recognized in earlier legislation but never implemented: they found that doctors should not be allowed to prescribe controlled substances: (1) for their own use; or (2) when not in “actual practice” (with an active medical license). Another provision that had been suggested in earlier regulations, but never implemented, was that all private prescriptions should be written on special forms. In 2006, the Misuse of Drugs Regulations were changed, and new arrangements made for prescribing controlled substances on special forms.13
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




