INSECT AND ARTHROPOD BITES
BEES, SPIDERS, SCORPIONS, AND OTHER SMALL BITERS
Bees, Wasps, Hornets, and Ants
“Killer bees” are an Africanized race of honeybees created by interbreeding of the African honeybee Apis mellifera scutellata (brought for experiments into Brazil) with common European honeybees. The hazard from these bees is that they tend to be more irritable, sense threat at a distance greater than their European counterparts, swarm more readily, defend their nests more aggressively and stay agitated around the nest for days, and impose mass attacks on humans. The venom of an Africanized bee is not of greater volume or potency than that of a European honeybee. However, the personality of the Africanized bees is such that they may pursue a victim for up to ⅔ mile (1 km), and may recruit other attacking bees by the hundreds or thousands. A victim may be stung from 50 to more than 1,000 times; it is estimated that 500 stings achieves the lethal threshold. The bees are established in Arizona, New Mexico, and California, and unfortunately appear to be increasing their habitat as they adapt to colder temperatures.
Treatment for Insect Sting
1. Be prepared to deal with a severe allergic reaction (see page 66). If the victim develops hives, shortness of breath, and profound weakness, and appears to be deteriorating, immediately administer epinephrine. This is injected subcutaneously (see page 474) in a dose of 0.3 to 0.5 mL for adults and 0.01 mL/kg (2.2 lb) of body weight for children, not to exceed 0.3 mL. Epinephrine is available in allergy kits with instructions for use. Anyone known to have insect allergies who travels in the wilderness should carry epinephrine. Take particular care to handle preloaded syringes carefully, to avoid inadvertent injection into a finger. When administering an injection, never share needles between people.
The drug is available in preloaded syringes in certain allergy kits, which include the EpiPen autoinjector and EpiPen Jr. autoinjector (Dey), the Twinject autoinjector (Verus: 0.3 mg or 0.15 mg doses; 2 doses per unit), and the Ana-Kit. Instructions for use accompany the kits. The EpiPen and Twinject epinephrine products are generally easier for laypeople to use, because they require less dexterity to accomplish injection with them. The Twinject autoinjector and Ana-Kit syringe are configured with enough epinephrine for a second (repeat) dose, which is sometimes necessary. The Twinject is a true autoinjector for the first dose; the second dose is delivered as a routine injection from a concealed syringe and needle.
2. Administer diphenhydramine (Benadryl) by mouth, 50 to 100 mg for an adult and 1 mg/kg (2.2 lb) of body weight for a child. This antihistamine drug may by used by itself for a milder allergic reaction. Topical antihistamine lotions or creams may be beneficial.
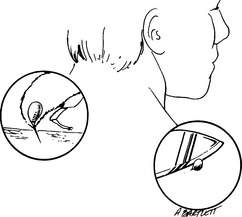
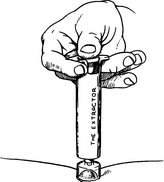
3. Stingers or pieces of stingers left in the skin should be removed as quickly as possible (Figure 203). It used to be taught that pulling the stinger out with fingers or forceps squeezed more venom into the victim, but this is currently not believed to be true. So, it is better to flick or pull a stinger and venom sac out of the skin of the victim using tweezers or your fingers than to waste precious time searching for a straight-edged object, such as a knife or credit card, to scrape away the stinger. Furthermore, crude scraping runs the risk of breaking off the stinger and leaving it embedded in the skin. An alternative is to try to pull out the stinger, then apply the Extractor device (Figure 204), if you are carrying one and it is available immediately after the sting has occurred.
4. Apply ice packs to the site of the sting.
5. Home topical remedies, such as aspirin, a 20% aluminum salt-containing preparation (including many household antiperspirants), or paste of baking soda or papain-containing meat tenderizer (such as Adolph’s unseasoned meat tenderizer) and water directly to the wound (for no more than 15 minutes), are of unproven value. Do not apply mud. The commercial product After Bite (Tender Corporation), a mixture of ammonium hydroxide and mink oil, is moderately effective for relief of pain and itching following insect bites, but will not abort an allergic reaction. StingEze liquid (Wisconsin Pharmacal) is a mixture of camphor, phenol, benzocaine, and diphenhydramine. This is a good agent to control itching and mild pain following any insect bite. Lidocaine 4% applied topically may help diminish discomfort.
6. If a person suffers an extensive skin and soft tissue reaction (swelling, itching, blisters), he may benefit from the administration of a corticosteroid, such as prednisone (60 mg by mouth day one, tapered by 10 mg per day over the next 5 days) or methylprednisolone (24 mg by mouth day one, tapered over the next 5 days).
7. If a person stung by an insect develops more than a mild to moderate local reaction, transport him to a hospital.
8. A bee sting in general does not pose a large risk for tetanus infection. Although deep punctures of other varieties deposit bacteria into the wound(s), where C. tetani can thrive in the absence of oxygen, a bee sting puncture isn’t that deep. The stinger might transfer bacteria from the skin surface, wherein lies the greatest risk. If a person has been immunized within the past 5 years, it is unnecessary to get a Td (or Tdap) booster immunization. If it has been more than 5 years but less than 10 years since the last tetanus shot, a Td (or Tdap) booster is indicated. If it has been more than 10 years since the last tetanus shot, both a Td (or Tdap) booster and tetanus immune globulin are indicated, if you go by the book.
Avoidance of Stinging Insects
1. Store garbage, particularly fruit, at a distance from the campsite.
2. Remove (carefully) beehives and wasp nests from children’s play areas.
3. Wear light-colored clothing. Dark-colored clothing is attractive to insects and may evoke a defensive (sting or bite) response. Keep shirt sleeves closed and tuck pants into boots. Wear light-colored socks.
4. Avoid wearing sweet fragrances that make you smell like a flower.
5. Do not anger bees or wasps. If confronted by a swarm, cover your face (eyes, nose, and mouth) and move rapidly from the area. If necessary, throw a blanket or towel over your head. Run if you must. Run through bushes or weeds to confuse the bees. Don’t jump into a pool—the bees may wait for you and a severe allergic reaction from a sting while in the water may be extremely dangerous. Do not poke sticks or throw rocks into bee holes.
6. Avoid rapid or jerky movements near bees. Do not swat at them.
SPIDERS
Black Widow Spider
In the United States, the female black widow spider (Latrodectus mactans) is about ⅝ in (15 mm) in body length, black or brown, and with a characteristic red (or orange or yellow) hourglass marking on the underside of the abdomen (Figure 205). The top side of the spider is shiny and features a fat abdomen that resembles a large black grape. The longest legs are directed toward the front. This species and other Latrodectus species are found scattered in rural regions, in barns, within harvested crops, and around outdoor stone walls. Some are arboreal.
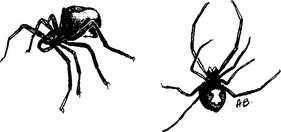
Figure 205 Female black widow spider with typical hourglass marking on the underside of the abdomen.
The bite of the black widow spider is rarely very painful (usually more like a pinprick) and often causes little swelling or redness, although there can be a warm and reddened area around the bite. If much venom has been deposited, the victim develops a typical reaction well within an hour. Symptoms include muscle cramps, particularly of the abdomen and back; muscle pain; muscle twitching; numbness and tingling of the palms of the hands and bottoms of the feet; headache; droopy eyelids; facial swelling; drooling; sweating; restlessness and anxiety; vomiting; chest muscle spasms, causing difficulty in breathing; fever; and high blood pressure. A man may develop a persistent penile erection (priapism). A small child may cry persistently. A pregnant woman may develop uterine contractions and premature labor.
Treatment for a Black Widow Spider Bite
1. Apply ice packs to the bite.
2. Immediately transport the victim to a medical facility.
3. Once the victim is in the hospital, the doctor will have a number of therapies to use, which include intravenous calcium solutions and muscle relaxant medicines for muscle spasm; antihypertensive drugs for elevated blood pressure; pain medicine; and, in very severe cases, antivenom to the venom of the black widow spider.
4. If you will be unable to reach a hospital within a few hours and the victim is suffering severe muscle spasms, you may administer an oral dose of diazepam (Valium), if you happen to be carrying it. The starting dose for an adult who does not regularly take the drug is 5 mg, which can be augmented in 2.5 mg increments every 30 minutes up to a total dose of 10 mg, so long as the victim remains alert and is capable of normal, purposeful swallowing. The starting dose for a child age 2 to 5 years is 0.5 mg; for a child age 6 to 12 years the starting dose is 2 mg. Total dose for a child should not exceed 5 mg; never leave a sedated child unattended.
Brown Recluse Spider
At least five species of recluse spiders are found in the United States. The brown recluse spider (Loxosceles reclusa) is the best known and found most commonly in the South and southern Midwest. However, interstate commerce has created habitats in many other parts of the country for the brown recluse and related species. The spider is brown, with an average body length of just under ½ in (10 mm). A characteristic dark violin-shaped marking (“fiddleback”) is found on the top of the upper section of the body (Figure 206). The brown recluse spider is found in dark, sheltered areas, such as under porches, in woodpiles, and in crates of fruit. It is most active at night. It commonly bites when it is trapped, but is not otherwise aggressive toward humans.

Figure 206 Brown recluse spider with typical violin-shaped marking on the top side of the cephalothorax.
The bite of the brown recluse spider may cause very little pain at first, or a sharp sting may be felt. The stinging subsides over 6 to 8 hours, and is replaced by aching and itching. Within 1 to 5 hours, a painful red or purplish blister sometimes appears, surrounded by a bull’s-eye of whitish-blue (pale) discoloration, with occasional slight swelling. The red margin may spread into an irregular fried-egg pattern, with gravitational influence, such that the original blister remains near the uppermost part of the lesion. The victim may develop chills, fever, weakness, and a generalized red skin rash. Severe allergic reactions within 30 minutes of the bite occur infrequently. Over 5 to 7 days, the venom causes a violet discoloration and breakdown of the surrounding tissue, leading to an open ulcer that may take months to heal. If the reaction has been severe, the tissue in the center of the wound becomes destroyed, blackens, and dies.
Treatment for a Brown Recluse Spider Bite
Until you receive other advice, treat the wound with a thin layer of mupirocin or bacitracin ointment, or mupirocin cream, underneath daily dressing changes. Do not apply topical steroids. Some persons have touted application of topical nitroglycerin, but there is not yet sufficient scientific evidence to routinely support this therapy.
Other Spiders
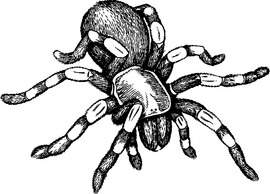
Some tarantulas (Figure 207) carry hairs that can irritate the skin, eyes, and mucous membranes of humans. When the spider is threatened, it rubs its hind legs over its abdomen and flicks thousands of hairs at its foe. These hairs can penetrate human skin and cause swollen bumps, which can itch for weeks. If any hairs or hair fragments remain in the skin, they can removed with repeated applications and peelings of sticky tape. After that, treatment is with an oral antihistamine and topical medication such as StingEze liquid. A topical antihistamine or corticosteroid preparation may provide some relief.
The hobo spider may cause a reaction similar to, but less severe than, a brown recluse spider. The bite wound should be treated accordingly (see page 380).
SCORPIONS
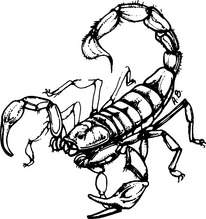
Scorpions are found in deserts and warm tropical climates, hidden under stones, fences, and garbage. In the United States, the most dangerous species is the nocturnal bark scorpion Centruroides exilicauda, which is found almost exclusively in the southwestern states and can be up to 2 in (5 cm) long. This yellowish-brown (straw-colored), solid or striped species is distinguished from other scorpions by its slender body and a small tubercle (telson) at the base of its stinger (Figure 208). The sting is inflicted with the last segment of the tail, and it is immediately exquisitely painful; the pain is made much worse by tapping on the site of the injury. Other symptoms include excitement, increased salivation, sweating, numbness and tingling around the mouth, nausea, double vision, nervousness, muscle twitching and spasms, rapid breathing, shortness of breath, high blood pressure, seizures, paralysis, and collapse. A child under age 2 years is at particular risk for a severe reaction. Stings by nonlethal scorpion species are similar to bee stings.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree