Summarized from: McLaughlin, L.A. and Braun, K.L. (1998). Asian and pacific islander cultural values: considerations for health care decision-making. Health and Soc Work, 23(2), 116–26.
Autonomous persons
The terms “capacity” and “competence” are both used to describe a group of capabilities necessary for decision-making. In the US, “capacity” usually is used by medical experts to describe functional capabilities, and “competence” is a legal term. In the United Kingdom, the usage is reversed, and “competence” usually refers to functional capacity, while “capacity” is a legal term.3 In this chapter the terms are used interchangeably.
Capacity is a “threshold” element in informed consent. Without the ability to make decisions, a person is not autonomous. Capacity is task specific: patients may be fully capable of making medical decisions even if they are unable to care for themselves in other ways. Capacity waxes and wanes depending on many factors such as the patient’s medical condition, psychological state, level of stress, and ability to orient to unfamiliar surroundings. Although any diagnosis of compromised mentation can interfere with competence, no diagnosis in a conscious patient invariably identifies incompetence. The presence of memory impairment, dementia, or mental illness, for example, does not prove a lack of capacity to make medical decisions.
Physician paternalism and bias pervades assessments of patient competence. Patients are often referred for competency evaluations simply because they refuse medical advice, although such refusals are not generally evidence of incapacity.4 In one study, noncompliant patients comprised almost two-thirds of referrals for competency evaluations, yet they were only slightly less likely than compliant patients to be judged incompetent by consultants. Patients who discharge themselves against medical advice from hospitals have a somewhat higher prevalence of alcohol abuse than the general population. However, studies have found that such actions are more often related to insurance status and lower income, or factors such as race (which might be associated with mistrust of physicians or
Table 1.2. Summary of patient rights to informed consent by country*
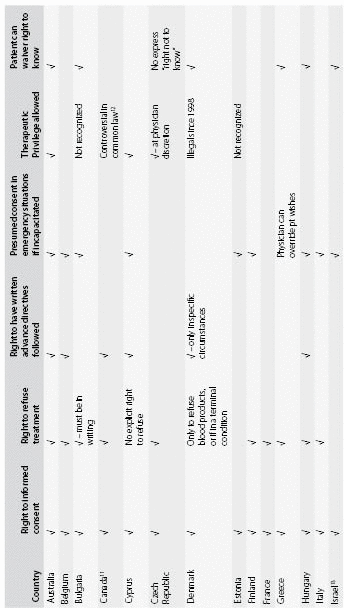

* Obtained from the Centre for Biomedical Ethics and Law unless otherwise noted http://europatientsrights.euandhttp://www.kuleuven.be
Spaces were left blank when there was no explicit provision in law according to the Centre for Biomedical Ethics and Law at the time of access to the website on March 1, 2010. Reader should note that provisions may nevertheless be implicit in other laws or regulations.
Spaces were left blank when there was no explicit provision in law according to the Centre for Biomedical Ethics and Law at the time of access to the website on March 1, 2010. Reader should note that provisions may nevertheless be implicit in other laws or regulations.
perceptions of disrespectful treatment) than to decisional incompetence.5
Physicians frequently judge patient competence based on their perception of the quality of a patient’s decision. A recent study of physicians’ attitudes toward patients who refuse cancer therapy found that physicians often regarded such decisions as “irrational,” and therefore reflecting mental aberrations.6 Such judgments place the physician’s own values, prejudices, and perceptions about medical treatment and quality of life before those of the patient, and do not reflect appropriate respect for patient autonomy. The same study found that patients refuse medical therapy based on personal values and experience more than on medical facts alone. Most experts believe that quality of life measures are at least equal in relevance to medical outcomes in determining if treatment results meet patient needs.
In general, competence to make medical decisions is adjudged to be present when the patient meets four criteria: they can communicate a choice, understand the relevant information, appreciate the medical consequences of the decision, and reason about treatment decisions (see also Chapter 4). These criteria generally can be assessed in pre-operative conversations with patients, and do not usually require expert consultation. When there is conflicting evidence about patient competence, however, a formal evaluation may be helpful.
The anesthesiologist in our introductory case made a hasty judgment about whether Allen was capable of participating in a complete discussion of options for his anesthesia care. An actual conversation with Allen would have revealed to her that he is employed, and lives independently – although these circumstances do not guarantee he has capacity for medical decision-making. When asked, he says that he needs to have surgery because of his sick intestines, and that he understands that he could get cancer if he does not have the operation. He also hopes that the surgery will reduce his pain and diarrhea. He does not fear anesthesia; he has been through several operations before without problems. Because of his religious beliefs he does not fear death. Allen appears to be an autonomous person with capacity to decide – or at least participate to a great degree – in decisions about his care, and should be given a complete description of his options in language aimed at his level of understanding.
Temporary incapacity
Many common clinical factors, both temporary and permanent, can impair the capacity to make medical decisions. Examples include severe pain or anxiety, intoxication, head injury, organic brain disease, developmental delay, and young age. Criteria for capacity in such patients, however, are no different from in any other situation. Physicians have ethical obligations to promote autonomy by treating patients to restore capacity if possible. Anxious patients or those suffering from pain ideally should have anxiety and pain treated prior to informed consent discussions, because they may then be better capable of listening to options, discussing information, and making decisions. Patients retain autonomy even with premedication if they are able to meet the four criteria cited above. Withholding such treatment until a consent form is signed is cruel, probably coercive, and may cause such consent to be legally invalid as well.
If delaying surgery allows a patient suffering from a temporary incapacity to recover competence in a time frame such that the surgery is still meaningful, the surgery should be postponed. If an emergency surgery cannot be delayed for a patient with temporary incapacity, then the physician may need to locate a surrogate decision-maker, or proceed without consent in the best medical interests of the patient.
Autonomous choices
Three conditions must be met in order for an act (or choice) to be autonomous: a person must act with intention, with understanding, and without controlling influences.
Intention
Ethical theory regarding “intention” is complex, but generally speaking intentional acts require “planning,” although not necessarily reflective thought or strategy. We do many things intentionally but without thought, such as reaching for a glass of water in order to drink, scratching an itch, or turning a page in a book.
Unintentional acts can result from accidents or habitual behavior, or even as a byproduct of an intentional act. Imagine that Mary presents with flank pain suggestive of a kidney stone. Her physician orders an intravenous pyelogram (IVP). After administration of the contrast agent and IV fluid, increased urine output washes the stone into the bladder. The IVP is negative, but Mary’s pain is resolved. The physician intended to run the test to diagnose the cause of her pain and he intended to appropriately treat the condition responsible for it. Both things happened. The test was run according to plan, but pain relief occurred because of an unintended side effect of the test. Mary’s pain relief was the result of an accident and not a result of intention, even though the outcome of the accident and the intended outcome of the physician’s plan are the same.
Patients are asked explicitly and implicitly to consent to both intentional and unintentional acts by physicians. Intentional acts are broadly categorized as those acts that result in the expected outcomes. Unintentional acts are those acts that result in outcomes that are not expected or not desired, such as side effects, accidents, and medical catastrophes. When autonomous patients consent following adequate information about both the known and intended, and known possible-but-unintended outcomes of treatment (and they are not manipulated or coerced), then they can be said to have intended to consent to the potential unintended consequences of treatment. It would be difficult to assert that a patient intended to consent to outcomes about which they were not informed. A patient who is inadequately informed is therefore not making an autonomous choice because intention is a requirement for autonomous choice. Adequate information is key to promoting patient autonomy, but what constitutes “adequate information”?
What the physician must disclose
It was not until the mid twentieth century that a legal obligation to inform patients prior to obtaining consent was established. In Salgo v Trustees of Leland Stanford Hospital7 it was found that physicians must discuss risks and alternatives to treatment, as well as describe the procedures and their consequences. This finding was reinforced in Canterbury v Spence in 1972, which determined:
… it is evident that it is normally impossible to obtain a consent worthy of the name unless the physician first elucidates the options and the perils for the patient’s edification.8
Physicians argued that the courts had imposed an impossible burden: explaining all of the possible risks and outcomes of procedures would be tantamount to providing the patient with a medical education. Patients were neither knowledgeable, nor educable to the level of detail needed to make “competent” medical decisions. Subsequent court findings disagreed. In Harnish v Children’s Hospital Medical Center, the duty to inform patients was further clarified:
A physician owes to his patient the duty to disclose in a reasonable manner all significant medical information that the physician possesses or reasonably should possess that is material to an intelligent decision by the patient whether to undergo a proposed procedure.9 [italics added]Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




