CHAPTER 172
Impetigo
Presentation
Parents will usually bring their children (most commonly aged 2 to 5 years) to be checked, because they are developing unsightly skin lesions. The lesions are usually painless but may be pruritic and are found most often on the face (Figure 172-1) or other exposed areas. Parents may be worried that their young child has “infant-tigo” (the common lay misnomer). Nonbullous lesions consist of irregular or somewhat circular red oozing erosions (sores), often covered with a yellow-brown honey-like crust (Figure 172-2). These may be surrounded by smaller erythematous macular or vesiculopustular areas. Bullous lesions (Figure 172-3) present as large thin-walled bullae, which quickly rupture and are replaced by a thin shiny varnish-like coating over the denuded area on an erythematous base. More than one area may be involved, and a mix of bullous and nonbullous findings can exist.
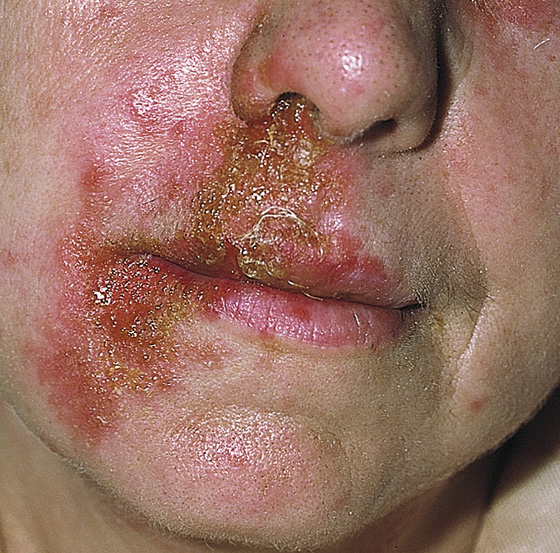
Figure 172-1 Impetigo of the face. (From White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
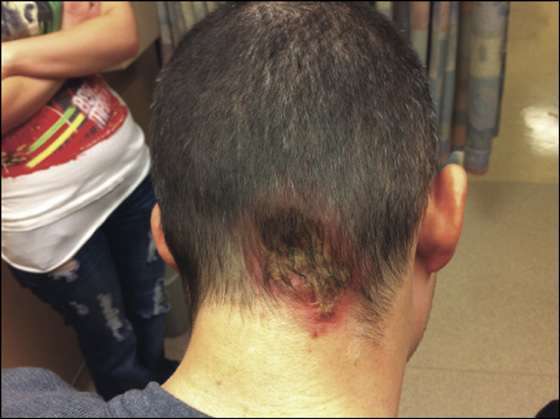
Figure 172-2 Kerion with surrounding impetigo.
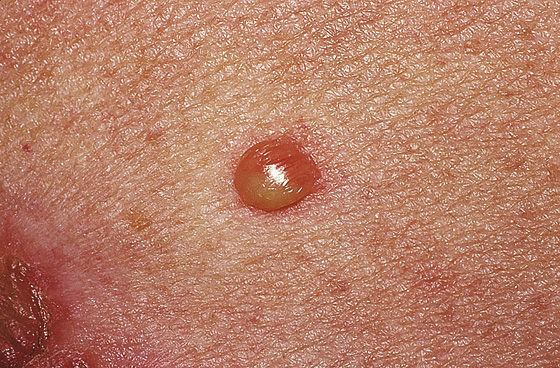
Figure 172-3 Bullous impetigo. (From White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
What To Do:
 For a few lesions involving a relatively small area, prescribe mupirocin 2% (Bactroban) cream or ointment to be applied to the rash tid for 10 days. Have parents soften and cleanse crusts with warm soapy compresses before applying the antibiotic cream or ointment. There is little scientific evidence regarding the value of any disinfecting measures, such as the use of povidone-iodine and chlorhexidine. A newer antibiotic, retapamulin (Altabax) (ointment 1% [available in 5-, 10-, and 15-g tubes], apply bid × 5 days), was approved by the Food and Drug Administration (FDA) in 2007 and although expensive, appears to be effective even against MRSA strains.
For a few lesions involving a relatively small area, prescribe mupirocin 2% (Bactroban) cream or ointment to be applied to the rash tid for 10 days. Have parents soften and cleanse crusts with warm soapy compresses before applying the antibiotic cream or ointment. There is little scientific evidence regarding the value of any disinfecting measures, such as the use of povidone-iodine and chlorhexidine. A newer antibiotic, retapamulin (Altabax) (ointment 1% [available in 5-, 10-, and 15-g tubes], apply bid × 5 days), was approved by the Food and Drug Administration (FDA) in 2007 and although expensive, appears to be effective even against MRSA strains.
 For large areas of involvement or resistant cases, add an oral antibiotic with activity against Staphylococcus aureus and group A beta-hemolytic streptococcal infections: azithromycin (Zithromax), 500 mg, then 250 mg qd (10 mg/kg, then 5 mg/kg/day) × 4 days, or cephalexin (Keflex), 250 to 500 mg tid to qid (25 to 50 mg/kg/day). Alternatives include amoxicillin/clavulanate (Augmentin), 250 to 500 mg/125 mg q8h (25 to 45 mg/kg/day divided q12h) × 10 days, or dicloxacillin, 250 to 500 mg qid (12.5 to 25 mg/kg/day divided q6h) × 10 days. In communities where community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) is prevalent, prescribe trimethoprim/sulfamethoxazole (Bactrim, Septra), 160 mg TMP bid (8 to 10 mg/kg/day divided q12h) × 10 days, or clindamycin (Cleocin), 150 to 300 mg qid (10 to 30 mg/kg/day divided q8h) × 10 days. Alternative options should be based on local susceptibility results.
For large areas of involvement or resistant cases, add an oral antibiotic with activity against Staphylococcus aureus and group A beta-hemolytic streptococcal infections: azithromycin (Zithromax), 500 mg, then 250 mg qd (10 mg/kg, then 5 mg/kg/day) × 4 days, or cephalexin (Keflex), 250 to 500 mg tid to qid (25 to 50 mg/kg/day). Alternatives include amoxicillin/clavulanate (Augmentin), 250 to 500 mg/125 mg q8h (25 to 45 mg/kg/day divided q12h) × 10 days, or dicloxacillin, 250 to 500 mg qid (12.5 to 25 mg/kg/day divided q6h) × 10 days. In communities where community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) is prevalent, prescribe trimethoprim/sulfamethoxazole (Bactrim, Septra), 160 mg TMP bid (8 to 10 mg/kg/day divided q12h) × 10 days, or clindamycin (Cleocin), 150 to 300 mg qid (10 to 30 mg/kg/day divided q8h) × 10 days. Alternative options should be based on local susceptibility results.
 Consider obtaining cultures if CA-MRSA is prevalent in your area.
Consider obtaining cultures if CA-MRSA is prevalent in your area.
 To prevent the spread of this infection, have the patient and his family wash their hands frequently, change towels and bed linens every day, and keep infected schoolchildren home until the acute phase has cleared. Nasal carriage of S. aureus has been implicated as a source of recurrent disease and can be reduced by the topical application of mupirocin within the nares twice daily for 5 days (nasal ointment 2% [1-g single-use tubes]); apply ½ tube in each nostril bid.
To prevent the spread of this infection, have the patient and his family wash their hands frequently, change towels and bed linens every day, and keep infected schoolchildren home until the acute phase has cleared. Nasal carriage of S. aureus has been implicated as a source of recurrent disease and can be reduced by the topical application of mupirocin within the nares twice daily for 5 days (nasal ointment 2% [1-g single-use tubes]); apply ½ tube in each nostril bid.
What Not To Do:
 Do not use bacitracin, neomycin, or similar antibacterial ointments on these lesions. They are less effective than mupirocin and may cause unnecessary contact dermatitis.
Do not use bacitracin, neomycin, or similar antibacterial ointments on these lesions. They are less effective than mupirocin and may cause unnecessary contact dermatitis.
Discussion
Impetigo is a common superficial skin infection that is mostly seen during the summer in temperate climates and throughout the year in warm, humid tropical regions worldwide.
Nonbullous impetigo was previously thought to be a group A streptococcal process, and bullous impetigo was primarily thought to be caused by S. aureus. Studies now indicate that both forms of impetigo are primarily caused by S. aureus, with Streptococcus usually being involved in the nonbullous form. If the infection is a toxin-producing phage group II type 71 Staphylococcus (the same toxin seen in scalded skin syndrome), large bullae will form as the toxin produces intradermal cleavage. Otherwise, smaller bullae develop, and the honey-crusted lesions predominate.
Impetigo is thought to be self-limiting, but studies on its natural history do not exist.
It is thought that antibiotic treatment does not alter the subsequent low incidence of secondary glomerulonephritis, especially in children aged 2 to 6 years. Presenting signs and symptoms of glomerulonephritis include edema and hypertension; about one third of patients have smoky or tea-colored urine.
Impetigo is very contagious among infants and young children and may be associated with poor hygiene, a break in the skin, or predisposing skin eruptions, such as herpes simplex, angular cheilitis, insect bites, scabies, and atopic and contact dermatitis. When lesions occur singly, they may be mistaken for herpes simplex. S. aureus can directly invade the skin and cause a de novo infection.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


