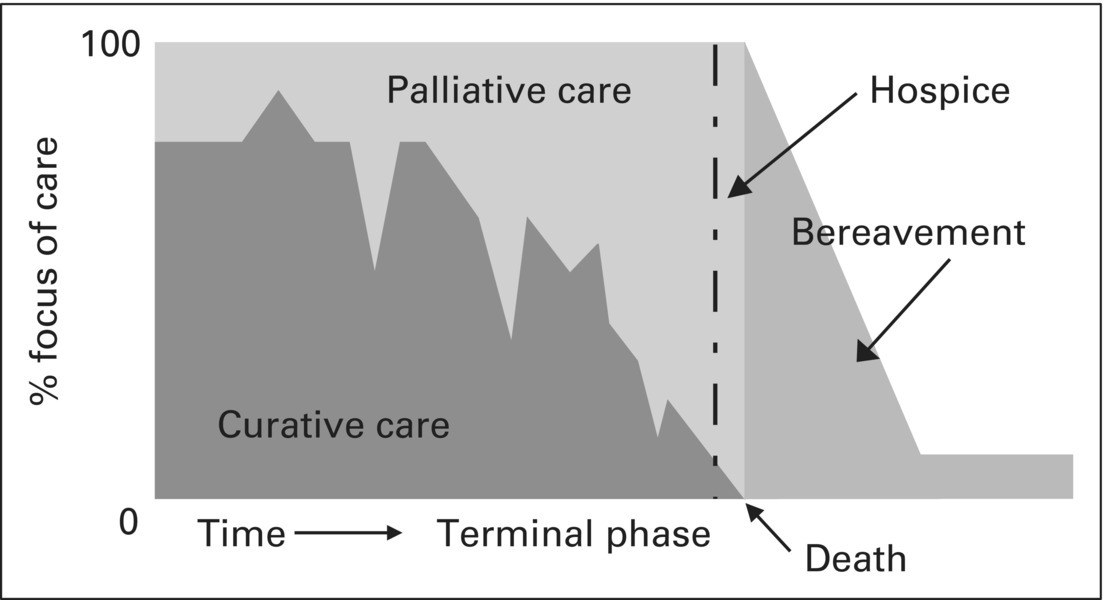
Chapter 1 Steven Z. Pantilat, Wendy G. Anderson, Matthew J. Gonzales, and Eric W. Widera Mrs Morton was an 82-year-old woman with ovarian cancer metastatic to the lung, liver, and peritoneum with massive ascites diagnosed 1 year ago. She had undergone many cycles of chemotherapy but stopped chemo several months ago due to progression of disease and increasing fatigue. Mrs Morton was living at home with her daughter, son-in-law, and three grandchildren. A few days earlier, she had stopped eating and drinking. She became sleepier and spent all of her time in bed. On the morning of admission, Mrs Morton’s daughter awoke to find that her mother was not able to speak or even open her eyes and was moaning and breathing fast. Feeling panicked, her daughter called 911. The ambulance arrived within a few minutes. They found Mrs Morton hypotensive, tachypneic, tachycardic, hypoxic, and in respiratory distress. They asked about advance directives, but were told that Mrs Morton had not completed one. They started an IV, gave fluids, administered oxygen, and rushed Mrs Morton to the hospital. On arrival in the emergency department, the emergency physician and nurse asked the family, “Would you like us to do everything possible?” Her family responded, “Yes,” as virtually anyone would to this question. The emergency physician called the hospitalist on call STAT to the emergency department to admit Mrs Morton and notified the intensive care unit that she would soon be on her way up. For hospitalists, intensivists, emergency physicians, advance practice nurses, nurses, and all clinicians who practice in the hospital, the story of Mrs Morton is all too common. Overall, about one-third of Americans die in hospitals; many more spend some time in a hospital in the last year of life [1]. Among Medicare beneficiaries, nearly 70% are hospitalized in the last 3 months of life, one-third receive ICU care in the last month of life, and over half die in a hospital or nursing home [2]. While it is arguable whether Mrs Morton needed hospital admission to receive quality care at the end of her life, as hospice or palliative care at home would likely have provided the care she needed, the reality is that for many people hospital care provides relief and recovery from exacerbations of chronic illness. People with acute shortness of breath from heart failure or chronic obstructive pulmonary disease (COPD), bowel obstruction from pancreatic cancer, altered mental status from liver failure, and pain from a pathologic fracture often experience rapid and dramatic improvement in symptoms and quality of life from hospital care. Even patients who prefer to avoid hospitalization may find that hospital care provides the quickest and best option for relief of symptoms. For example, Chapter 4 discusses options for treating patients with malignant bowel obstruction. In this clinical setting, hospitalization may offer the best option for relief of nausea, vomiting, and pain. At the same time, for a patient like Mrs Morton, there will likely come a time when hospitalization will not only fail to provide relief but may also impose additional burdens for her and her family. Although it can be difficult to predict which hospitalization will be the last one or whether hospitalization will provide more benefit than harm, each hospitalization for the seriously ill provides an opportunity to clarify goals of care to ensure that care is consistent with patient preferences, promotes benefit, and limits harm. Studies of patients with serious illness have shown consistently what these patients need and want from the healthcare system: relief from pain and other symptoms; clear communication about their illness, prognosis, and treatment options; and psychosocial, spiritual, and practical support [3, 4]. Addressing these needs is critical for providing high-quality care to patients with serious illness, and as such provides the overarching organizational structure to this book. Further, it requires a team approach as no single clinician has expertise in all these domains. Hospitalists and other hospital-based physicians, nurses, social workers, and chaplains must collaborate to ensure that patient needs are attended to. Such collaboration can happen formally, as with a palliative care consultation team, or more informally through clinicians working together to share insights and develop and implement plans of care. Increasingly, it is hospitalists and other hospital-based specialists who care for people with serious illness in the hospital like Mrs Morton [5]. Over time, hospitalists have come to care not only for people with classic medical conditions, such as pneumonia and COPD, but also for people with cancer and cardiac, neurologic, and surgical problems either as admitting physicians or through comanagement. The high frequency of hospitalization among the seriously ill and those approaching the end of life places the clinicians who work in these settings in an ideal position to promote optimal quality of life for these patients. Palliative care is the field of medicine focused on providing the best possible quality of life to people with serious illness and those near the end of life. Palliative care is defined as follows: …specialized medical care for people with serious illnesses. This type of care is focused on providing patients with relief from the symptoms, pain, and stress of a serious illness—whatever the diagnosis. The goal is to improve quality of life for both the patient and the family. Palliative care is provided by a team of doctors, nurses, and other specialists who work with a patient’s other doctors to provide an extra layer of support. Palliative care is appropriate at any age and at any stage in a serious illness, and can be provided together with curative treatment. [6] There are several important parts of this definition that bear highlighting. First, palliative care is for people with serious illnesses. While palliative care is also about caring for people near and at the end of life such as Mrs Morton, fundamentally, palliative care is for people with serious illnesses such as heart disease, COPD, cirrhosis, cancer, and dementia and would have been appropriate for Mrs Morton from the time of diagnosis. The term serious illness is also helpful when talking with patients about the need for palliative care or the decision to involve palliative care specialists. Patients can easily relate to and understand that they have a serious illness and that additional care will be helpful to them. In the hospital, palliative care will also be appropriate for patients with fulminant acute illness such as massive intracranial hemorrhage and trauma. The important point for hospitalists to remember is that palliative care is not only for the terminally ill and also for those at the very end of life. Palliative care is also appropriate at any stage in a serious illness, and patients can receive palliative care while still pursuing curative intent treatment such as chemotherapy, radiation therapy, percutaneous coronary interventions, surgery, and hemodialysis. Many patients and physicians harbor the misconception that receiving palliative care means that patients must forsake curative intent treatment. This misunderstanding is a common barrier that unnecessarily precludes patients from receiving palliative care. Patients admitted with exacerbations of heart failure or COPD, with complications of cancer or its treatment, and those with dementia all may benefit from symptom management, clarification of goals of care, and psychosocial support. One helpful question to ask for determining whether a patient would benefit from palliative care is, “Would I be surprised if this patient died in the next year?” This “surprise” question helps clinicians identify patients appropriate for palliative care [7]. If the question is difficult to apply to every patient, clinicians can also consider the types of patients who would be appropriate for palliative care (Table 1.1). Table 1.1 Types of Patients Appropriate for Palliative Care Consistent with what patients say they need from the healthcare system, palliative care seeks to relieve the symptoms, pain, and stress of a serious illness. Relief of symptoms and pain is the first priority as patients can only focus on what is important to them and on having meaningful time when their symptoms are controlled. Control of symptoms allows patients to consider the issue that is at the heart and the ultimate goal of palliative care: improving quality of life. In fact, one helpful way to explain palliative care to patients and families is to state that the goal is to help patients “achieve the best possible quality of life for as long as possible.” This focus on promoting quality of life and understanding that it is defined uniquely by each patient is at the crux of what palliative care is about. It is also helpful to explain to patients that palliative care provides an extra layer of support. Few hospitalized patients would decline extra support, and the more seriously ill the patient, the more attractive and necessary the extra support becomes. Hospitalized patients fall along a continuum of an illness trajectory, and palliative care plays a significant role in the care of patients throughout this continuum. The needs of these patients with serious illness will vary over the course of illness, and as shown in Figure 1.1, the relative focus on palliative care and curative intent treatment may change. Similarly, the depth and intensity of involvement with palliative care concerns will change over time, but from diagnosis to death, patients with serious illness will encounter situations where they will need and benefit from palliative care. Figure 1.1 Concurrent model of palliative care. Source: © Steven Pantilat, MD and Regents of the University of California.
Hospital Care for Seriously Ill Patients and Their Families
1.1 EPIDEMIOLOGY OF HOSPITAL CARE FOR THE SERIOUSLY ILL
1.2 PALLIATIVE CARE
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





