Anesthesia Techniques and Monitors
The effect of neuromuscular blockade on mask ventilation
Warters RD, Szabo TA, Spinale FG, et al (Med Univ of South Carolina, Charleston) Anaesthesia 66:163-167, 2011§
Evidence Ranking
• A
Expert Rating
• 2
Abstract
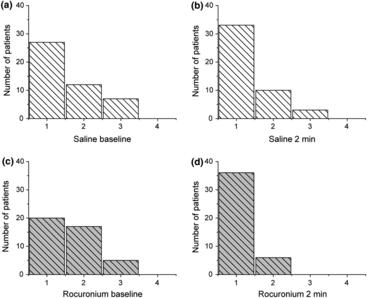
We wished to test the hypothesis that neuromuscular blockade facilitates mask ventilation. In order reliably and reproducibly to assess the efficiency of mask ventilation, we developed a novel grading scale (Warters scale), based on attempts to generate a standardised tidal volume. Following induction of general anaesthesia, a blinded anaesthesia provider assessed mask ventilation in 90 patients using our novel grading scale. The non-blinded anaesthesiologist then randomly administered rocuronium or normal saline. After 2 min, mask ventilation was reassessed by the blinded practitioner. Rocuronium significantly improved ventilation scores on the Warters scale (mean (SD) 2.3 (1.6) vs 1.2 (0.9), p < 0.001). In a subgroup of patients with a baseline Warters scale value of > 3 (i.e. difficult to mask ventilate; n = 14), the ventilation scores also showed significant improvement (4.2 (1.2) vs 1.9 (1.0), p = 0.0002). Saline administration had no effect on ventilation scores. Our data indicate that neuromuscular blockade facilitates mask ventilation. We discuss the implications of this finding for unexpected difficult airway management and for the practice of confirming adequate mask ventilation before the administration of neuromuscular blockade (Fig 1).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree