CHAPTER 165
Diaper Dermatitis
(Diaper Rash)
Presentation
Irritant Diaper Dermatitis
An infant, most commonly between 8 and 10 months of age, may be left too long between diaper changes or, during a diarrheal illness, develops irritation and erythema that is most evident on the prominent parts of the buttocks, medial thigh, and vulva or scrotum. Margins are not always evident. There may be papules or small superficial erosions, and skin folds are spared or involved last (Figure 165-1).
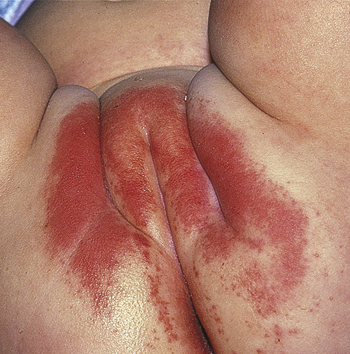
Figure 165-1 Irritant diaper dermatitis. (Adapted from White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
Candidal Diaper Dermatitis
Following a course of antibiotics, a mild diaper rash may suddenly worsen, with clusters of erythematous papules and pustules coalescing into a beefy red confluent painful rash with sharp borders that are surrounded by small satellite lesions. The skin folds are commonly involved (Figure 165-2).
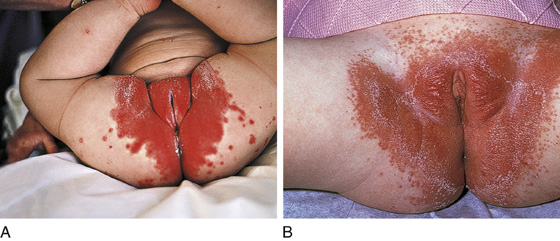
Figure 165-2 Two examples of Candida diaper rash. (Adapted from White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
What To Do:
 For a mild irritant rash, recommend frequent diaper changes (the most important intervention) and have the parents avoid excessive rubbing, especially with baby wipes that contain alcohol or fragrance, which may actually add to the irritation. Have the parents rinse the baby’s bottom with clear water at each diaper change. They can use a sink, tub, or water bottle for this purpose. Gentle cleansing with soft moist washcloths and cotton balls also can be helpful. Have them pat the baby dry rather than rubbing her down with a towel.
For a mild irritant rash, recommend frequent diaper changes (the most important intervention) and have the parents avoid excessive rubbing, especially with baby wipes that contain alcohol or fragrance, which may actually add to the irritation. Have the parents rinse the baby’s bottom with clear water at each diaper change. They can use a sink, tub, or water bottle for this purpose. Gentle cleansing with soft moist washcloths and cotton balls also can be helpful. Have them pat the baby dry rather than rubbing her down with a towel.
 Tell the parents to loosen their baby’s diapers or use oversized diapers to allow airflow and prevent chafing at the waist and thighs.
Tell the parents to loosen their baby’s diapers or use oversized diapers to allow airflow and prevent chafing at the waist and thighs.
 They may also apply a barrier over-the-counter (OTC) agent such as petroleum jelly (Vaseline), A and D Ointment, Triple Paste, Diaperene, Desitin, or Balmex. Zinc oxide is the active ingredient in many diaper rash creams. These products are usually applied in a thin layer to the irritated region several times throughout the day.
They may also apply a barrier over-the-counter (OTC) agent such as petroleum jelly (Vaseline), A and D Ointment, Triple Paste, Diaperene, Desitin, or Balmex. Zinc oxide is the active ingredient in many diaper rash creams. These products are usually applied in a thin layer to the irritated region several times throughout the day.
 For a more severe or persistent rash, also instruct the parents to allow the child to go “bare” and wear no diapers as much as possible, but especially at nap time, until the rash has healed. To avoid messy accidents, the parents may try laying the baby on a large towel and engaging her in some playtime while going bare-bottomed. This may increase the laundry load, but it allows the skin to dry, avoids physical trauma, and restores natural defenses.
For a more severe or persistent rash, also instruct the parents to allow the child to go “bare” and wear no diapers as much as possible, but especially at nap time, until the rash has healed. To avoid messy accidents, the parents may try laying the baby on a large towel and engaging her in some playtime while going bare-bottomed. This may increase the laundry load, but it allows the skin to dry, avoids physical trauma, and restores natural defenses.
 These more severe cases will also benefit from the application of an OTC 1% hydrocortisone cream or ointment bid.
These more severe cases will also benefit from the application of an OTC 1% hydrocortisone cream or ointment bid.
 For a mild candidal infection, or for a diaper rash lasting more than 3 days, have the parents apply a topical antifungal cream or ointment, such as 2% miconazole (Micatin), 1% clotrimazole (Lotrimin), 2% ketoconazole (Nizoral), or 1% naftifine after each diaper change.
For a mild candidal infection, or for a diaper rash lasting more than 3 days, have the parents apply a topical antifungal cream or ointment, such as 2% miconazole (Micatin), 1% clotrimazole (Lotrimin), 2% ketoconazole (Nizoral), or 1% naftifine after each diaper change.
 With increased inflammation, a combination antifungal-steroid agent, such as triamcinolone/nystatin (Mycolog II), can be applied bid.
With increased inflammation, a combination antifungal-steroid agent, such as triamcinolone/nystatin (Mycolog II), can be applied bid.
 For a severe Candida diaper rash, or if there is oral thrush, perianal candidiasis, or repeated bouts of candidal infection, prescribe oral treatment with nystatin to clear the gastrointestinal tract. Use nystatin oral suspension (60-mL bottle, 100,000 units/mL), 4 to 6 mL PO qid, 2 mL qid for infants.
For a severe Candida diaper rash, or if there is oral thrush, perianal candidiasis, or repeated bouts of candidal infection, prescribe oral treatment with nystatin to clear the gastrointestinal tract. Use nystatin oral suspension (60-mL bottle, 100,000 units/mL), 4 to 6 mL PO qid, 2 mL qid for infants.
 Recommend the same local measures as noted previously for irritant diaper rash.
Recommend the same local measures as noted previously for irritant diaper rash.
 For secondary bacterial infection (e.g., crusting, vesicles, bullae), prescribe mupirocin (Bactroban) 2% ointment tid for 10 days. For severe infections, a broad-spectrum systemic antibiotic, such as amoxicillin/clavulanate (Augmentin), will be required.
For secondary bacterial infection (e.g., crusting, vesicles, bullae), prescribe mupirocin (Bactroban) 2% ointment tid for 10 days. For severe infections, a broad-spectrum systemic antibiotic, such as amoxicillin/clavulanate (Augmentin), will be required.
 Encourage parents to practice hand washing after changing diapers to prevent the spread of bacteria or yeast to other parts of their baby or to other children.
Encourage parents to practice hand washing after changing diapers to prevent the spread of bacteria or yeast to other parts of their baby or to other children.
 Make sure that the family has a pediatrician or family practitioner for further follow-up.
Make sure that the family has a pediatrician or family practitioner for further follow-up.
What Not To Do:
 Do not recommend talcum powder or “talcum-free” powders for use when diapers are changed. They add little in terms of medication or absorbency and are occasionally aspirated by infants as their diapers are being changed.
Do not recommend talcum powder or “talcum-free” powders for use when diapers are changed. They add little in terms of medication or absorbency and are occasionally aspirated by infants as their diapers are being changed.
 Do not recommend using cornstarch to protect the baby’s skin. Cornstarch helps promote the growth of yeast and bacteria.
Do not recommend using cornstarch to protect the baby’s skin. Cornstarch helps promote the growth of yeast and bacteria.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


