CHAPTER 8 DELIVERING MULTIDISCIPLINARY TRAUMA CARE: CURRENT CHALLENGES AND FUTURE DIRECTIONS
The origins of trauma care delivery are deeply rooted in the major military conflicts of the last century. During the Napoleonic Wars, Dominique Larrey established the concepts of field hospitals, the use of the “flying ambulances” and the principles of triage.1 In World War I, rapid and timely evacuation of the injured from the battlefield through echelons of treatment facilities, each with increasing surgical capabilities, became the standard of care.2 During World War II, in addition to reducing the time from evacuation to treatment, the principle of “resuscitation” or treatment of shock prior to transport evolved. When combined with the other advances in transfusion technology, surgical technique, antibiotics, and so on, this systematic approach to trauma care resulted in a significant decrease in mortality. This approach was further refined in the Korean conflict and the Vietnam War, when wounded soldiers were rapidly transported within minutes by helicopter to fully capable hospitals, where the entire spectrum of trauma care from initial resuscitation to definitive surgical management was delivered.3 Experience gained in the battlefield allowed large, urban medical centers to develop similar paradigms of trauma care for victims of “urban warfare.” However, in spite of extensive training, these same trauma surgeons were unable to provide the same level of care outside these urban hospitals. Therefore, it became clear that the system, and not the individuals, were responsible for the observed successes, and the need for trauma systems, not just trauma surgeons, became recognized.
The publication of the seminal report, Accidental Death and Disability: The Neglected Disease of Modern Society, in 1966 became the catalyst in changing the delivery of trauma care. This report highlighted the magnitude of the problem in both human and economic terms and lack of an organized public or governmental response to the problem. As this became a major political issue, Congress responded by enacting the National Highway Safety Act of 1966. The resultant funding spurred the development of trauma systems in the states of Maryland, Florida, and Illinois. Additional federal funding followed passage of Titles 18 and 19 of the Medicare and Medicaid Act, the Emergency Medical Services Systems Act of 1973, and the Emergency Medical Services Amendments of 1976. Prompted by perceived financial gains, a large number of hospitals sought designation as “trauma centers.” With the sharp decline in funding following the Omnibus Budget Reconciliation Act of 1981, the exodus of participating institutions was as rapid as their entry into the system. The specialty care of trauma then became the purview of centers that retained an interest in caring for victims of traumatic injury in spite of the disadvantages that are associated with doing so.4
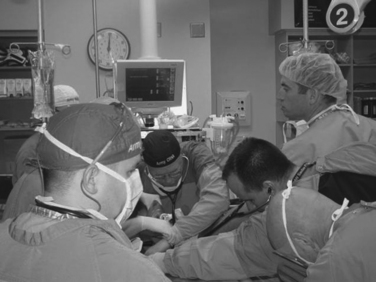
Over the ensuing years, trauma systems have matured with the trauma center as their cornerstone. Adequately addressing the issue of traumatic injury is recognized to include a spectrum beginning with injury prevention and education, throughout the immediate acute care phase, and extending into the rehabilitation. The success of these systems is recognized in the ability of trauma centers, in the context of trauma systems, to reduce mortality and morbidity. Further, lessons learned are being applied in the theater of war. Medical teams on the front lines of battle in Iraq and Afghanistan are receiving training prior to deployment at select trauma centers and employing principles refined in the civilian sector (Figure 1).
In spite of this compelling evolution, the delivery of trauma care continues to face significant challenges (Table 1). Technological advances of the last decade have increased the complexity of care, and require a multidisciplinary approach for an optimal outcome. Such an approach is associated with increasing costs, which in the face of skyrocketing malpractice premiums and declining reimbursements, challenges the financial health of trauma centers. Increased involvement of multiple specialists makes the logistics of providing adequate emergency room coverage and coordination of care a potentially daunting task. The workforce of trained trauma surgeons is shrinking as new graduates from general surgery training programs see trauma, in all but select programs, as a predominantly nonoperative specialty.
Table 1 Key Challenges to Multidisciplinary Delivery of Trauma Care
| Financial | Increasing costs |
| Skyrocketing malpractice premiums | |
| Declining reimbursements | |
| Multispecialty care | Emergency room coverage |
| Coordination of care | |
| Shrinking workforce | Limited trained trauma surgeons |
| Restricted resident work hours | |
| Reduced operative experience | |
| Special considerations | Nutritional support |
| Substance abuse | |
| Neuropsychological support | |
| Rehabilitation | |
| Placement | |
| Special populations | Children |
| Pregnant women | |
| Elderly | |
| Funding | Educational outreach activities |
| Research |
In order to overcome these challenges, we need to redefine the philosophy of trauma surgery and trauma surgeons. The purpose of this review is to describe efforts that are currently under way and other potential solutions currently being entertained to optimize patient care.
ORGANIZING THE INITIAL CARE OF TRAUMA PATIENTS
Prehospital Communication
Direct communication between the trauma center and emergency medical personnel is key.5 The heads-up on the nature and number of arriving trauma victims along with the estimated time of arrival allows for better preparation of required personnel and equipment. This becomes more relevant when multiple casualties are involved, and team members of varying levels of experience are designated according to patients’ severity of injuries. In specific circumstances, it also allows certain specialists to be called in even before the patient arrives (e.g., the neurosurgeon for a traumatic quadriplegia). Activation of “surge capacity” procedures for mass casualty events can be done with the maximum lead time.6 In addition, medical direction can be provided to prehospital personnel in cases outside the realm of those in standard operating procedures.
Tiered Trauma Team Activation
Patients meeting trauma criteria result in activation of a trauma alert. The full complement of providers arrives at the resuscitation bay after being notified. The time before actual patient arrival is utilized to determine what is known about the patient, the likely interventions required, and to reaffirm roles. Members of such a team include the trauma surgeon, trauma fellow/senior surgical resident, junior surgical resident, trauma nurses, physician assistant (PA) anesthesiologists, respiratory technician, and radiology technician. Our current criteria for a trauma alert are enumerated in Table 2. Evaluation and management then follows the principles of the Advanced Trauma Life Support (ATLS) protocols.
Table 2 Trauma-Alert and High-Index Criteria
| Adult Trauma Alert Criteria | |
| Red criteria | Active airway assistance required |
| Blood pressure <90 systolic or no radial pulse with sustained heart rate >120 | |
| Multiple long-bone fractures | |
| 2nd- or 3rd-degree burns ≥body surface area, amputation proximal to wrist or ankle, penetrating injury to head, neck, torso | |
| Glasgow Coma Scale <12 | |
| Paramedic judgment | |
| Blue criteria | Sustained respiratory rate ≥30 |
| Sustained heart rate ≥120 with radial pulse | |
| Single long-bone fracture due to motor vehicle accident or fall ≥10 feet | |
| Major degloving, flap avulsion >5 inches, gunshot wound to extremities | |
| Best motor response = 5 | |
| Ejection from vehicle (excluding open vehicles) or deformed steering wheel | |
| Age 55 or older | |
| High-Index Criteria | |
| Falls ≥12 feet in adults, and ≥6 feet in children | |
| Extrication time >15 minutes | |
| Rollover | |
| Death of an occupant in the same vehicle | |
| Major intrusion | |
| Ejection from a bicycle | |
| Pedestrian struck by a vehicle | |
| Age 55 or greater | |
| Paramedic judgment |
Note: Presence of one red or two blue criteria constitutes a trauma alert.
For patients with traumatic injuries who do not meet trauma criteria, the designation “high index” is applied. These patients are taken directly to the emergency department (ED). They undergo a similar and thorough trauma work-up under the direction of the ED physician. Once the work-up has been completed, a consultation with the trauma service is obtained. The team reviews findings and the plan of care, and arranges for the necessary follow-up.
On occasion, a high-index patient will be found to have significant injuries or comorbidities that exceed the abilities of the ED physician or the capabilities of the ED. On such occasions, an in-house trauma alert is called, the patient transferred to the resuscitation bay, and the entire team rapidly assembled. Availability of this safety net allows the ED to increasingly participate in the management of the injured. It also reduces the workload imposed on an already busy trauma service, and decreases the costs of an otherwise full activation. It is, however, associated with a more prolonged ED stay, but does not result in suboptimal outcome.7,8
In-House Trauma Attending
It is being increasingly recognized that trauma outcomes are directly related to institutional commitment and not just to the experience of the individual surgeon.9,10 As such, the need for the presence of the trauma attending has been challenged. Attending presence, however, has certain definite advantages. Patient disposition can be more rapid, with real-time interpretation of diagnostic studies and front-end decision making, bypassing the traditional approach of communication along progressive echelons of command. Coordination with other specialists becomes easier with direct attending-to-attending discussions. In institutions where trauma patients may be admitted to services other than the trauma service (e.g., the orthopedic service for isolated orthopedic injuries or the neurosurgical service of isolated neurological injury), the patient may be appropriately arbitrated to the service that will serve the patients interest best. Presence of an in-house trauma attending allows this arbitration to be made after careful consideration of the patient’s trauma burden, preventing admission of trauma patients to nonsurgical services. Finally, attending presence allows for the provision of billing for services, including the initial evaluation and management, surgeon-performed ultrasonography, tube thoracostomy, vascular access lines, and so on.
Captain of the Ship Concept
Over the last two decades, there has been explosive increase in the modalities available for the management of complex injuries.11 The emphasis has been on the development of nonoperative and minimally invasive strategies that involve interventional radiologists and endovascular surgeons, among others.12 Additionally, nontraditional stakeholders such as anesthesiologists (e.g., epidural catheters for pain management in rib fractures) and endoscopists (e.g., endoscopic retrograde cholangiopancreatography/papilotomy for complex liver trauma with bile leaks) are now becoming key players in delivering care.13,14 It is of paramount importance, therefore, to have strong leadership in the trauma service serving as the “captain of the ship,” guiding the patient’s care through the nuances of the various available options, while at the same time, protecting the patient from the need or desire to “push the envelope.”
Trauma Coverage by Specialists
The provision of emergency coverage by specialists has been, and continues to be a major challenge.15,16 On the one hand, tertiary hospitals must provide specialist coverage or risk potential loss of substantial federal and state funding for their trauma centers. At the same time, use of hospitalists to relieve specialists of admissions and the development of alternative venues of practice (e.g., ambulatory surgery centers) have encouraged some specialists, once dependent on hospitals, to reduce or drop their clinical privileges. Change of privilege status from active to courtesy is becoming an increasingly popular option in avoiding provision of emergency coverage. This is further compounded by the skyrocketing malpractice premiums.
Radical changes will be necessary to overcome this problem. Some of the potential solutions to improving emergency coverage by specialists are enumerated in Table 3. Another alternative is to incorporate training of basic emergency procedures used in these specialties into the core trauma curriculum. The dependence on specialties may be reduced with an orthopedic trauma rotation focused on irrigation and debridement of open fractures and application of external fixators, along with a neurosurgical rotation focusing on placement of intracranial monitoring devices, decompressive craniotomies, and evacuation of space occupying lesions, such as subdural or epidural hematomas.17 The ability to provide trauma care on a more elective basis may be appealing and result in increased involvement. It is also our experience that maintaining the care of the patient on the trauma service serves as a strong incentive to motivate participation.
Table 3 Potential Solutions to Improve Emergency Coverage by Surgical Specialists
| Outsource coverage to corporations of multispecialty groups. |
| Pay emergency availability stipend to specialists. |
| Work together at local, state, and federal levels to obtain funding for uninsured or partly insured patients. |
| Establish working networks with hospitals within the jurisdiction to minimize unnecessary transfers and prevent EMTALA violations. |
| Make community leaders aware of the crisis in emergency specialcare through the ist coverage to facilitate a designated tax increase for provision of stipends. |
| Establish a fair on-call schedule among the different specialists. |
| Hospitals need to recognize that the days for free emergency coverage in lieu of maintaining clinical privileges are over. |
| Emergency coverage needs to be a key part when negotiating managed care contracts. |
| Increase the number of hospitalists to reduce the admission burden for specialists. |
| Create additional sources of funding for trauma centers (red light violations, speeding tickets, dedicated taxes, etc.). |
EMTALA, Emergency Medical Treatment and Labor Act.
ORGANIZING SUBSEQUENT CARE OF TRAUMA PATIENTS
Role of Tertiary Survey
Despite due diligence, the potential for missed injuries exists.18–20 The presence of a low Glasgow Coma Scale (GCS) on admission, or the need for pharmacologic paralysis, limits the accuracy of the physical examination, significantly increasing this risk. The most common reason for a missed injury is an inadequate clinical examination. The majority of missed injuries can be identified on repeat clinical assessment with the appropriate imaging studies, especially when a high index of suspicion is maintained. When present, these injuries add to the morbidity and mortality with a less than optimal outcome. It is our routine for the trauma attending to perform a tertiary survey for all patients admitted for more than 24 hours. The task may alternatively be delegated to the trauma surgery fellow or senior surgical resident. It must, however, be performed in all admitted patients, at the prescribed time and in a thorough manner. It includes a complete physical examination and review of all radiological studies.21 Any detected abnormality can be addressed appropriately, with the necessary interventions taken.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree