CHAPTER 39 Critical Care Medicine
Critical illness occurs in stages. The acute illness is followed by a plateau phase, which may be prolonged and is poorly understood. The biphasic response to stress exhibited by the hypothalamic pituitary adrenal axis is also poorly understood. In critically ill patients, an initial surge in adrenocorticotropic hormone (ACTH) and cortisol is followed by a prolonged state of decreased ACTH levels and persistently elevated cortisol (Beishuizen and Thijs, 2004). Persistent hypercortisolism may benefit the patient by promoting the availability of fuel substrates and minimizing inflammation, or it may be harmful, causing hyperglycemia, delayed wound healing, immune suppression, and myopathy. The immune or inflammatory response to injury follows a similar pattern (Hotchkiss and Karl, 2003).
An increasing number of studies have focused on long-term functional outcomes, and these are likely to change critical care practice in coming years. For example, although tolerance of relative hypoxia has become the norm for treating patients with acute respiratory distress syndrome (ARDS), outcome studies show that duration of saturation less than 90%, less than 85%, and less than 80% correlated with impairment in memory, attention, and processing speed, respectively (Hopkins et al., 1999). Pediatric patients undergoing arterial switch, a procedure that should leave them with normal long-term heart function, had a higher than expected incidence of neurodevelopmental disabilities at school age (Mehta and Arnold, 2004). As more information about how to promote good long-term functional outcomes becomes available, our practice will evolve.
Respiratory system
Actual or impending respiratory failure is a common reason for admission to the PICU, and one in six patients admitted requires mechanical ventilation (Epstein, 2009). Although some patients with healthy lungs require mechanical ventilation for nonrespiratory reasons, the majority have acute respiratory failure due to lung parenchymal disease. The treatment of acute respiratory failure remains primarily supportive. The goal of treatment is to avoid further damage to the lungs and other organ systems during the period required for the lungs to heal.
Modes of Mechanical Ventilation in the PICU
Support Modes
Effort above a preset rate may or may not be supported. The most common form of support is pressure support. Pressure support has been shown to facilitate weaning, and it may also improve patient comfort. Pressure support is frequently used to recondition weakened respiratory muscles while still providing mandatory breaths to prevent atelectasis; however, data to support this approach do not exist (Turner and Arnold, 2007).
Noninvasive Positive Pressure Ventilation
Over the past few years, there has been an increase in the use of noninvasive ventilation to prevent or delay endotracheal intubation. Noninvasive positive pressure ventilation (NPPV) includes continuous positive airway pressure (CPAP), which is used to increase functional residual capacity (FRC) and to overcome inspiratory airway collapse, and biphasic positive airway pressure, which also supports respiratory effort with positive inspiratory pressure. Studies in adults have shown clear benefit to NPPV, especially when endotracheal intubation can be avoided, with no decrement when endotracheal intubation is merely delayed (Pagano and Barazzone-Argiroffo, 2007). NPPV has been demonstrated successfully in pediatric patients with neuromuscular disease, upper airway obstruction, status asthmaticus, and cystic fibrosis (Deis, 2008).
Ventilator-Induced Lung Injury
Ventilator-induced lung injury is caused by prolonged exposure to high Fio2, by alveolar stretch from excessive tidal volumes (volutrauma), and by opening and closing of alveoli (shear stress trauma). Although hyperoxic inspired gas is essential for patients with lung injury, exposure to Fio2 greater than 95% for 24 to 48 hours causes lung injury similar to ARDS and causes death within 48 to 72 hours due to oxygen toxicity (Adams et al., 2003).
Mechanical trauma from ventilation causes injury both through physical disruption of the architecture of the lung and through release of inflammatory mediators. Atelectatrauma, which is thought to occur when PEEP is set below the lower inflection point of the lung hysteresis curve, is particularly problematic in lung disease states associated with surfactant dysfunction, such as ARDS. Patients with heterogeneous lung disease are at increased risk for volutrauma. Transpulmonary pressure is not uniformly distributed to alveoli, and collapsed alveoli adjacent to inflated alveoli may be subject to extreme shearing forces. Mechanical trauma leads to release of inflammatory mediators, which may spill over to systemic circulation and play a role in the development of multiorgan failure (Plötz et al., 2004; Harris, 2005; Tremblay and Slutsky, 2006).
Use of Lung Hysteresis Curves
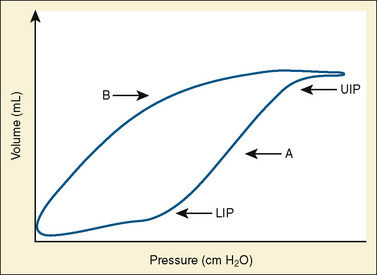
More sophisticated ventilators can calculate pressure-volume loops showing the difference in the pressure-volume relationship between the inspiratory and expiratory limbs of the respiratory cycle (Fig. 39-1). The sigmoidal shape of the hysteresis curve reflects differing compliance at different lung volumes. The lower inflection point represents the point during inspiration at which compliance improves. Below this point, the majority of alveoli are closed. The upper inflection point represents another change in compliance. Above a certain volume, more pressure is required to further distend alveoli, and the upper inflection point is thought to represent the beginning of a zone in which further pressure causes significant alveolar strain. The curve is steepest and nearly linear between these points, reflecting maximal compliance. Lung injury is thought to be minimized by keeping PEEP above the lower inflection point to maintain recruitment, and keeping tidal volumes below the upper inflection point by minimizing peak inspiratory pressure (Tremblay and Slutsky, 2006).
Alternative Modes of Ventilation
High-Frequency Oscillatory Ventilation
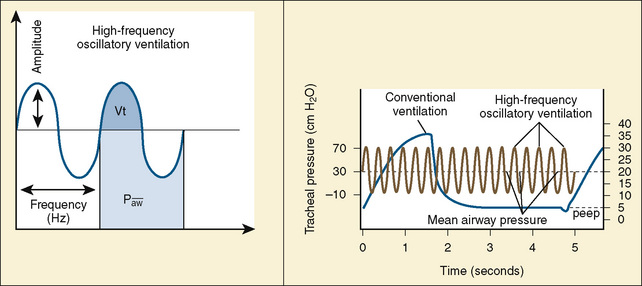
Despite conventional ventilation strategies to reduce VILI, about one third of patients with ARDS die, and many of the survivors experience a significant decrement in function. The object of high-frequency oscillatory ventilation (HFOV) is to accomplish oxygenation and ventilation with less injury to the lung. HFOV uses laminar flow at high MAPs to maintain the lung open, and it uses an oscillating piston to create pressure displacement above and below the MAP to deliver very small tidal volumes in the range of the volume of the patient’s anatomic dead space (Stawicki et al., 2009) (Fig. 39-2). The result, ideally, is ventilation only on the steep and linear part of the hysteresis curve. Compliant alveoli, which might receive an excessively large share of the delivered tidal volume in conventional ventilation, are protected from volutrauma. With this strategy, noncompliant alveoli—those with time constants long enough to preclude opening with conventional ventilation—may be recruited. Recruitment of new lung units may improve V/Q matching. A crossover trial comparing HFOV with conventional ventilation in children with severe lung disease showed that HFOV was associated with improved oxygenation and, despite higher MAPs, a reduced need for supplemental oxygen at 30 days (Arnold et al., 1994).
In HFOV, the variables controlled on the ventilator are frequency of respiration, (measured in cycles per second, or Hertz), amplitude of ventilation (power), and MAP. Frequency is measured in cycles per second. A frequency of 10 is 600 “breaths” per second, and a frequency of 3 is 180 breaths per second. A lower frequency functionally creates a longer inspiratory time and therefore a larger breath. The frequency is initially set at 10 for infants, and somewhat lower for older children. Amplitude, also referred to as power, is measured in centimeters of water. There is no standard starting pressure. The amplitude is initially set to produce a visible wiggling motion of the patient’s body to the level of the lower abdomen or groin. MAP is initially set to 5 cm H2O greater than the last MAP on conventional ventilation (Stawicki et al., 2009). A chest radiograph performed within an hour or two after initiating HFOV should confirm an appropriate MAP setting by showing approximately nine visible ribs from the top of the thorax to the diaphragm.
Ventilation can be improved by increasing the amplitude and decreasing the frequency. As the frequency of breaths decreases, a higher percentage of the set amplitude will be delivered. This is like increasing the tidal volume in a conventional ventilator; decreasing frequency is a way to increase ventilation, thereby decreasing Paco2. Frequencies less than 3 (180 cycles per minute) may increase the risk for volutrauma (Stawicki et al., 2009).
For a more complete treatment of the mechanics of HFOV, see Stawicki and colleagues (2009).
Airway Pressure-Release Ventilation
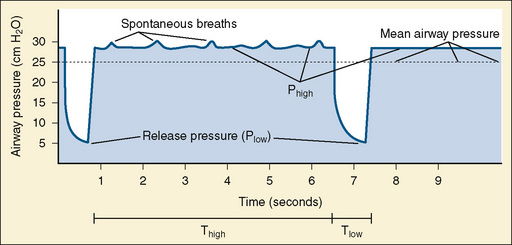
Airway pressure-release ventilation (APRV) cycles between a high- (Phigh) and a low-pressure level (Plow) in a high-flow CPAP circuit (Fig. 39-3). The continuous high flow allows spontaneous breathing throughout the ventilatory cycle, and it may reduce the need for heavy sedation and neuromuscular blockade. Spontaneous breathing is necessary to realize the benefits of this mode of ventilation (Stawicki et al., 2009).
Most of the respiratory cycle is spent at Phigh, and pressure is briefly released to Plow several times per minute. Ideally, time spent at Phigh will maximize recruitment and, by placing the lung on the steep part of the hysteresis curve, make spontaneous breathing easier. The time spent at Plow allows ventilation, but it is believed to be brief enough to prevent atelectasis of alveoli with long time constants (Stawicki et al., 2009).
Initially, Phigh is set at the plateau pressure measured from an inspiratory pause on conventional ventilation and adjusted to allow weaning of Fio2. Plow is set at zero to maximize the velocity of exhalation. The time (T) of Thigh is initially set between 4 to 6 seconds and adjusted to maintain adequate oxygenation and ventilation. Tlow is set at 0.4 to 0.5 seconds and adjusted to maintain a tidal volume of about 5 mL/kg, or such that expiration ends when the flow reaches 50% to 75% of the measured maximal expiratory flow. Tlow is the critical variable that affects bulk air flow and thus ventilation. Oxygenation is increased by increasing Fio2 or by increasing Phigh or Thigh, both of which will increase MAP. Ventilation is increased by encouraging spontaneous respiration or increasing Tlow (Stawicki et al., 2009).
Although it was described in 1987, APRV is relatively new in pediatrics and has not been thoroughly studied. Case reports of APRV in pediatric patients have shown improvement in oxygenation with the ventilation strategy (Krishnan and Morrison, 2007; Kuruma et al., 2008). With a crossover design, the one randomized controlled trial of APRV in children demonstrated comparable ventilation at lower peak inspiratory and plateau pressures (Schultz et al., 2001). The potential advantages of decreasing mechanical ventilatory pressures and allowing spontaneous breathing and a reduced need for sedation and neuromuscular blockade in patients with severe lung disease make it worth considering despite the paucity of data. APRV may be contraindicated in patients with severe obstruction to exhalation, such as status asthmaticus.
Adjuncts to Mechanical Ventilation for Patients with Severe Lung Disease
Helium-Oxygen Mixtures (Heliox)
Helium is a low-density, biologically inert gas that can be safely mixed with oxygen. When air flow through a tube is turbulent, the flow rate depends on the density of the gas. With high helium concentrations, heliox can flow more rapidly through narrowed airways than nitrogen-oxygen mixtures. Additionally, carbon dioxide diffuses through helium faster than through air. The Fio2 required by the patient may limit the use of heliox, as minimal benefit is believed to occur from heliox concentrations of less than 60%. When used with a spontaneously breathing patient, efforts should be made to prevent entrainment of room air with a well-fitting nonrebreather mask. Heliox can be delivered through the ventilator but may interfere with tidal volume measurements. This difficulty can be overcome with in-line monitors of respiratory mechanics (Myers, 2006).
Heliox may improve the delivery of nebulized medications. It improves dyspnea and peak expiratory flow in spontaneously breathing asthmatics, and it may limit peak inspiratory pressure in ventilated patients with status asthmaticus (Gupta and Cheifetz, 2005; Kissoon et al., 2008). Heliox improves respiratory distress associated with upper airway obstruction and improves the work of breathing in patients with bronchiolitis (Gupta and Cheifetz, 2005). No adverse effects of heliox have been reported. Despite a widespread belief that early application of heliox can prevent the need for intubation in select patients, there are no studies of heliox directed at patient outcomes.
Prone Positioning
In a supine patient, the dependent lung is underventilated and at risk for collapse, and the antidependent lung is aerated and at risk for overdistention. The mechanism by which prone positioning can improve oxygenation is not completely clear, but it may improve V/Q matching by improving the aeration of the dependent lung (Ryu et al., 2008). Prone positioning can also improve lung mechanics by decreasing thoracoabdominal compliance. In adult patients, a protocol of prone positioning for 7 hr/day improved oxygenation but did not alter ventilator-free days or mortality (Gattinoni et al., 2001). In pediatric patients, a protocol of prone positioning for 20 hr/day improved efficiency of oxygenation but did not improve ventilator-free days or organ failure–free days (Curley et al., 2005).
Nitric Oxide
Inhaled nitric oxide (iNO) has been a mainstay of treatment for both primary and secondary pulmonary hypertension of the newborn since its introduction. In these patients, it causes a rapid and sustained improvement in efficiency of oxygenation by preferentially vasodilating ventilated lung units (Konduri and Kim, 2009). Because it is rapidly inactivated by hemoglobin, the effect of iNO is limited to the pulmonary vasculature (Adhikari et al., 2007).
Because the pathophysiology of ARDS and acute lung injury (ALI) involves V/Q mismatching, there has been interest in using iNO for patients outside the neonatal age range. In adult studies, iNO improved oxygenation (i.e., the ratio of pulmonary arterial oxygen pressure [Pao2] to Fio2, and the oxygenation index) but did not improve mortality. There has been some concern in adult patients that iNO may be associated with an increase in the need for new renal replacement therapy (Adhikari et al., 2007). In a randomized trial in children, iNO improved oxygenation without harmful side effects from methemoglobinemia at dosages up to 20 parts per million. The study was not powered to detect a difference in mortality (Tang et al., 1998).
Nitric oxide is commonly used at a level of 20 ppm. Very high concentrations of NO may paradoxically worsen V/Q matching by diffusing into nonventilated areas and improving the perfusion there. High concentrations also carry a significantly increased risk for methemoglobinemia. Methemoglobin should be monitored daily while therapy with iNO is used. If methemoglobin becomes elevated, it is usually sufficient to decrease the concentration of iNO. For very high methemoglobin levels, a scavenger, such as methylene blue, may be used. Exposure to NO for even a brief period can sensitize the pulmonary vasculature to its effects. Rapid weaning to low levels (5 ppm) is usually well tolerated, but thereafter, iNO should be weaned slowly to prevent rebound vasoconstriction (Adhikari et al., 2007).
Surfactant
Surfactant deficiency has been described in ARDS and ALI, particularly in the acute phase of the illness. The best-studied application of surfactant is in meconium aspiration syndrome, where significant clinical improvement is reported after surfactant instillation (Willson et al., 2008). Surfactant instillation in infants mechanically ventilated for respiratory syncytial virus disease leads to improvement in oxygenation and decrease in duration of mechanical ventilation (Tibby et al., 2000; Luchetti et al., 2002).
Trials of endotracheal instillation or aerosolization of surfactant in adults have shown little or no benefit. In children, treatment with calfactant, a natural preparation relatively rich in surfactant specific protein B, has been associated with improved oxygenation and mortality, with particular benefit seen in patients younger than 12 months (Willson et al., 2005). Although this trial generated significant interest in the use of calfactant for pediatric ARDS and ALI, an independent analysis of the data noted that the placebo arm of the trial had more immunocompromised patients, and that statistical significance was lost when controlling for immune status (Czaja, 2007). Surfactant therapy for ARDS/ALI in patients outside of the neonatal age range remains controversial.
Surfactant is administered by direct endotracheal instillation through an endotracheal tube or bronchoscope at a dosage of 100 mg/kg body weight. The total volume of the drug preparation is significant. Complications of surfactant instillation include volume-responsive hypotension and transient hypoxia. Most authors cite pulmonary hemorrhage as a relative contraindication (Willson et al., 2008). Surfactant is probably best used early in the course of mechanical ventilation. Administration of surfactant in patients with severe hypoxia can provoke severe desaturation. In patients with severe hypoxia, surfactant may be safely given while the patient is supported with extracorporeal therapies.
Weaning and Extubation
Not all patients require gradual weaning. An alternative approach is to perform a daily test of extubation readiness, such as a spontaneous breathing trial, and give higher amounts of support to provide periods of rest for the respiratory muscles between these tests. A third approach is to provide periods of rest interspersed with periods of lower support designed to exercise or train the muscles of respiration. Several adult studies have shown that protocolized weaning results in earlier extubation without an increase in complications (Newth et al., 2009). Studies of weaning protocols in children are ongoing. Pediatric studies have corroborated adult data showing that spontaneous breathing trials with a T-piece (i.e., a tracheotomy tube collar) or pressure support can predict successful extubation (Newth et al., 2009). A negative inspiratory force of –30 correlates with extubation success in adults but has not been validated in children.
Despite weaning and careful testing, 8% to 20% of patients fail extubation. Extubation failure is independently associated with a fivefold increased risk for mortality in children, and upper airway obstruction accounts for or contributes to 25% to 40% of extubation failures (Newth et al., 2009). Testing for a leak around the endotracheal tube may predict post-extubation stridor, particularly in patients with uncuffed endotracheal tubes and those whose intubation has been prolonged. The absence of a leak at 30 cm H2O does not accurately predict extubation failure, but it is commonly a trigger for the use of steroids. Dexamethasone given 24 hours in advance of extubation may reduce the inflammation associated with airway injury from the endotracheal tube (Randolph, 2009).
Specific Disease Processes Requiring Mechanical Ventilation
Asthma
NPPV, if applied early in patients with status asthmaticus, can take advantage of patient’s respiratory efforts and prevent the muscle fatigue that leads to the need for intubation (Stather and Stewart, 2005). There is evidence that NPPV prevents hospitalization in patients presenting to the emergency department with status asthmaticus. Mental status changes, anxiety, exhaustion, or refractory hypoxemia preclude the use of NPPV, and it is these clinical changes rather than arterial blood gas analysis results that should guide the decision to intubate.
Once the patient is intubated, the primary strategy is to limit gas trapping, which causes intrinsic PEEP and forces the lung to operate on the less compliant portion of the hysteresis curve. Gas trapping is evident in flow-versus-time graphs, where inspiration is seen to start before flow returns to zero, or in graphs of end-tidal CO2 versus time, where CO2 fails to reach a plateau before the next inspiration begins (Stather and Stewart, 2005).
Significant controversy exists as to the best method for ventilating asthmatics. There are advocates for both pressure- and volume-control ventilation. Because of the high air-flow rates required to achieve targeted pressure in pressure-control ventilation, this mode may cause more turbulence in the airways of ventilated asthmatics. Volume-control modes may require higher set pressures to deliver adequate tidal volumes; however, because much of the pressure is lost in overcoming proximal airway resistance, alveolar hyperinflation may not occur. Alveolar pressure can be measured with an inspiratory pause pressure; complications are rare when this pressure does not exceed 30 cm H2O (Stather and Stewart, 2005).
Intrinsic PEEP can be measured with an expiratory pause pressure in a muscle-relaxed patient. Because complete exhalation is the goal, some authors recommend minimizing PEEP with an initial setting from 0 to 5 cm H2O. Others, acting on the theory that PEEP will stent airways open and ameliorate gas trapping, recommend setting PEEP at or slightly higher than the measured intrinsic PEEP. If a higher-PEEP strategy is used, intrinsic PEEP should be measured frequently, and the ventilator settings should be adjusted accordingly (Stather and Stewart, 2005).
There is general agreement that exhalation time should be as long as possible. Low respiratory rates and short inspiratory times give maximum exhalation time, but often at the expense of minute ventilation. Permissive hypercapnia (see Acute Respiratory Distress Syndrome and Acute Lung Injury, next) has been successfully used in the ventilation of asthmatics (Stather and Stewart, 2005). With permissive hypercapnia, patient ventilatory dyssynchrony is common. Neuromuscular blockade with adequate sedation is often necessary until severe bronchospasm resolves, usually within 24 hours. Weaning and extubation should be prompt, because spontaneous respiration is favorable for asthmatics. There are no generally agreed on criteria for extubating asthmatics, except that it should be performed as soon as possible. Negative inspiratory pressure with active exhalation is more effective than positive pressure in obstructive lung disease. Blood gas and ventilatory parameters that suggest the patient with asthma is improving include a normalizing partial pressure of CO2 and pH, and a peak inspiratory pressure that begins to approach the inspiratory pause pressure. The difference between peak inspiratory pressure and inspiratory pause pressure correlates with airway resistance.
Acute Respiratory Distress Syndrome and Acute Lung Injury
The clinicopathologic picture of ARDS and ALI is diffuse alveolar damage, and four clinical parameters are involved: acute onset, severe arterial hypoxemia resistant to supplemental oxygen, bilateral infiltrates, and absence of left atrial hypertension. A Pao2/Fio2 ratio of less than 200 mm Hg defines ARDS, and a ratio of less than 300 mm Hg defines ALI (Randolph et al., 2003).
The most common cause of ARDS and ALI is lower respiratory tract infection, but it can be precipitated by a variety of systemic inflammatory conditions, including infection outside the respiratory tract, pancreatitis, and tissue necrosis. Overall mortality for children ranges between 8% and 15%, which is lower than that for adults (Randolph et al., 2003). Patients with bone marrow transplantation may have a significantly higher mortality. Because of the low mortality in children, duration of mechanical ventilation or number of ventilator-free days are both considered acceptable endpoints for studies of ARDS and ALI.
Although not a predictor of mortality in adults with ARDS, multiple single-center and multicenter studies of the epidemiology of ARDS and ALI in pediatric patients confirm that the ratio of the alveolar oxygen pressure (Pao2) to Fio2 at the onset of ARDS or ALI is an independent predictor of mortality (Flori et al., 2005; Erickson et al., 2007). Mortality rates for children with ARDS or ALI from studies in the past 10 years range from 8% to 35% (Willson et al., 2008; Randolph et al., 2003). A recent prospective multicenter observational study of 320 children with ARDS or ALI found that mortality in patients with a Pao2/Fio2 ratio of less than 200 is nearly twice the mortality in those with a ratio between 200 to 300 (26% versus 13%) (Erickson, 2007). The Pao2/Fio2 ratio also predicted the number of ventilator-free days (Flori et al., 2005). The severity of hypoxia is also sometimes measured by the oxygenation index, defined as (MAP × Fio2)/Pao2 (Randolph, 2009).
Treatment of ARDS and ALI
Control of a persistent trigger of the inflammatory cascade is critical to eliminating the stimulus for ongoing lung injury. Because inflammation with capillary leak is part of the pathophysiology of ARDS, patients may benefit from a restrictive fluid strategy (Wiedemann et al., 2006). Fluid restriction should be initiated only after a patient with shock has been adequately resuscitated. Treatment of hypoproteinemia with albumin and furosemide may also be beneficial (Randolph, 2009).
Intensive care unit (ICU) stays for patients with ARDS or ALI may be prolonged, so is important to be attentive to other organ systems and to the prevention of iatrogenic injury. Strategies to avoid ICU-related pneumonia, critical care myopathy, central line infection, deep venous thrombosis, and gastritis, will be discussed later (see Prophylaxis).
Mechanical ventilation strategies for ARDS and ALI are designed to minimize VILI while protecting the patient from profound hypoxia. A Pao2 target of 55 to 80 mm Hg (i.e., an arterial oxygen saturation as measured by pulse oximetry [SpO2] of 88% to 95%) is commonly recommended for adult patients but may be too low for children, as the effect of prolonged marginal oxygenation on the developing brain is unknown. Most authors recommend an SpO2 target of greater than 90% for children (Randolph, 2009).
Alveolar collapse is possible with a low tidal volume strategy. Recruitment maneuvers with such a strategy include application of a sustained increase in airway pressure (i.e., a pressure of 40 mm Hg for 40 seconds) with a goal of opening the collapsed lung. After recruitment, PEEP is optimized to maintain the open lung (Randolph, 2009).
Permissive Hypercapnia
If the mode of ventilation that maintains ideal oxygenation and minimizes VILI is not capable of adequate CO2 exchange, a lower pH and a higher Pco2 may be tolerated. Patients in whom hypercapnia is being tolerated to minimize lung stretch will exhibit increased air hunger and anxiety and will require increased sedation. Hypercapnia is accompanied by acidosis in the acute phase, until renal compensation can buffer the pH. Hypercapnic acidosis (HCA) may benefit patients with ARDS or ALI apart from its association with ventilator strategies designed to decrease lung stretch. HCA increases cardiac output and organ blood flow (Rogovik and Goldman, 2008). It has antiinflammatory effects and attenuates free radical production. It may thus function to attenuate further lung injury from mechanical ventilation and from evolving infection.
HCA may have deleterious effects in select populations. Decreases in neutrophil chemotaxis and in the bactericidal activity of neutrophils and macrophages seen with HCA may be harmful, particularly in patients with sepsis (Curley et al., 2010). HCA increases pulmonary vascular resistance, and therefore it may not be appropriate for patients who are anticipated to have reactive pulmonary vasculature, particularly those in the neonatal age range (Curley et al., 2010). The increase in organ blood flow with HCA can cause increased intracranial pressure (ICP) in at-risk patients. Higher levels of CO2 are not believed to damage the brain, but rigorous long-term outcome studies in children have not been done (Curley et al., 2010).
Extracorporeal Membrane Oxygenation
Despite all the innovative therapies, deterioration of lung function in patients with acute respiratory failure may lead to a requirement for 100% oxygen and high ventilatory pressures. In some of these patients, extracorporeal membrane oxygenation (ECMO) can ensure adequate oxygenation and ventilation without high Fio2 and without potentially injurious airway pressures, allowing time for the lungs to heal. ECMO has been a particularly effective treatment for neonates with persistent pulmonary hypertension of the newborn: the use of ECMO reduced mortality in this group from between 80% and 85% to about 20% (Roy et al., 2000). Although older trials had suggested that ECMO for acute respiratory failure in adults was futile, the Extracorporeal Life Support Organization registry reports a survival rate of 53% for the small number of adult patients treated with ECMO for respiratory failure (Zapol et al., 1979; Conrad et al., 2005). A recent randomized trial of ECMO for adults with acute respiratory failure found the therapy effective in terms of improving survival without disability, and in terms of cost effectiveness (Peek et al., 2009). The use of ECMO was associated with an improved survival in pediatric patients with respiratory failure (Green et al., 1996). In pediatric patients, the mortality reported by the Extracorporeal Life Support Organization registry was 56% (Conrad et al., 2005). A randomized controlled trial of ECMO in pediatric patients was attempted but failed because of an overall decrease in mortality, probably resulting from lung-protective ventilation strategies.
The general indication for ECMO is reversible lung disease that prevents adequate oxygenation with conventional therapy, or shock refractory to medical treatment in a patient who is believed to have reversible disease (see ECMO for Circulatory Support of the Patient with Shock, later).
It is difficult to precisely identify the indications for ECMO for the patient with respiratory failure. The issue is clearer in neonates, who may be expected to have a relatively rapid resolution of pulmonary hypertension and a good outcome with extracorporeal therapy. Before the advent of high-frequency oscillating ventilation and nitric oxide, an oxygenation index of 40 was the criterion for considering ECMO. A recent review of 174 newborns with respiratory failure suggested that using a lower oxygenation index (the authors suggested 33.2) as the criterion for ECMO resulted in a lower mortality rate and a lower rate of chronic lung disease (Bayrakci et al., 2007). As mechanical ventilation becomes more sophisticated, it becomes more difficult to identify its moment of failure. With continuous innovation, it is also difficult to collect historical data for criteria that would identify patients in whom mortality with conventional ventilation exceeds the expected mortality with ECMO.
ECMO should be considered in a patient with high airway pressures and high Fio2 who may be expected to require a long course of mechanical ventilation, or when the clinician believes that the probability of chronic lung disease induced by mechanical ventilation outweighs the risk of ECMO. The best outcomes are seen in patients with single-organ dysfunction and viral pneumonia. Mortality is highest in patients with trauma, immune suppression, or multiple-organ dysfunction syndrome (MODS) at the time of ECMO initiation. Most authors consider prolonged ventilatory course (>10 to 14 days) with high pressures and high Fio2 to contraindicate ECMO, because significant VILI has already occurred (Frenckner and Radell, 2008). Survival to hospital discharge is less likely in patients who have been ventilated longer than 10 days (Nehra et al., 2009). Absolute contraindications to ECMO include conditions that make cannulation impossible, including severe prematurity or small size (e.g., infants <34 weeks old and weighing <2 kg), any condition that would preclude systemic heparinization (e.g., major coagulopathy, active hemorrhage, or recent intracranial hemorrhage), or conditions amenable to surgical repair (e.g., total anomalous pulmonary venous return and lethal anomalies).
The pulmonary hypertension that leads to neonates requiring ECMO resolves in a few days, but the lung damage that leads to pediatric patients requiring ECMO is much slower to heal. For pediatric patients, the mean time on ECMO is almost 2 weeks (Frenckner and Radell, 2008; Nehra et al., 2009). A recently published 8-year experience with ECMO from Massachusetts General Hospital described an average duration of ECMO for respiratory failure of 274 hours (11.4 days), with a range of 1 to 1154 hours (48 days) (Nehra et al., 2009). The duration of a course of ECMO should be considered on a case-by-case basis. In general, it is reasonable to continue ECMO support for a pediatric patient with respiratory failure until there is clear evidence that pulmonary disease is irreversible, or until complications preclude survival.
Every day on ECMO increases the risk for complications. Bleeding occurs in up to 16% of pediatric patients on ECMO, and it is most commonly seen at surgical sites, at cannula sites, and in the GI tract. Complications related to the ECMO circuit (e.g., oxygenator failure, cannula dysfunction, tubing rupture, pump malfunction) occur for 14% of pediatric patients (Frenckner and Radell, 2008). During prolonged ECMO runs, attention to the support and preservation of extrapulmonary organ systems becomes paramount. Patients who may require ECMO should be sent to a center with expertise in the procedure before the severity of lung disease prevents safe transport.
For a thorough review of management of the patient on ECMO, see Frenckner and Radell (2008). For the most complete resource on ECMO management, see Van Meurs and colleagues (2005).
Cardiovascular system
Treatment of shock is the mainstay of emergent support of the cardiovascular system in the pediatric ICU. It is difficult to determine what percentage of shock seen in pediatric patients presenting to the PICU is septic shock, because nearly three fourths of children admitted to the PICU meet the criteria for systemic inflammatory response syndrome (SIRS) (Carvalho et al., 2005; Wessel and Laussen, 2006). Therefore, recommendations for treatment of shock are skewed toward SIRS, probably the most common cause of shock in the PICU. Despite their disparate causes, the various types of shock share a common pathophysiology and treatment, and classifying shock by etiology is not particularly useful in children. Pediatric patients with septic shock present with elements of hypovolemic, cardiogenic, and distributive shock (Zanotti-Cavazzoni and Dellinger, 2006).
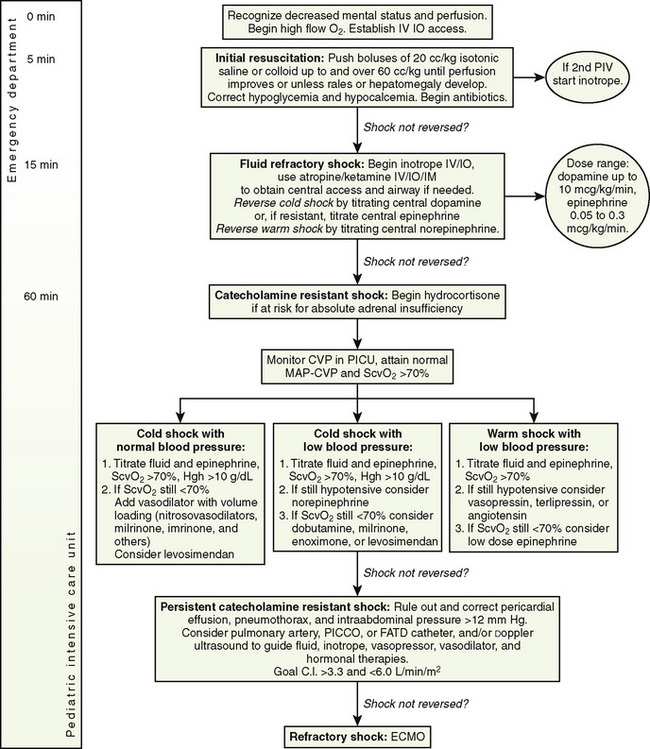
Rapid resuscitation and management of shock are critical to the treatment of children with shock, and diagnosing the type of shock is secondary to initiating resuscitation (Brierley et al., 2009). Aggressive fluid resuscitation and initiation of inotropes and antibiotics should be accomplished within the first hour after presentation. In adults, an early and aggressive protocol for septic shock has proved vastly more effective than any pharmacologic intervention (Rivers et al., 2001). Pediatric shock resuscitation protocols call for symptomatic treatment of shock using clinical signs as endpoints. The guidelines are divided into specific tasks to be accomplished in the first 5 minutes, the first 15 minutes, and the first hour (Fig. 39-4). The guidelines from the American College of Critical Care Medicine (ACCM) have resulted in improved outcomes for children with septic shock (Han et al., 2003; de Oliveira et al., 2008).
Recognition of Shock and Initial Resuscitation
Outcomes are improved if shock is recognized by its early signs, before the onset of arterial hypotension (Han et al., 2003). Because of children’s capacity to increase systemic vascular resistance, they may be normotensive in shock. Tachycardia is a sensitive but nonspecific indicator. Prolonged capillary refill in a central location, particularly when combined with tachycardia, is a more specific indicator of shock. Once the diagnosis of shock has been made, resolution of tachycardia is a useful indicator of successful treatment. Severe tachycardia (>180 beats/min in a child younger than 1 year, or >140 bpm in a younger child) in a severely ill child may be rapidly followed by a precipitous decline in blood pressure (Dabrowski et al., 2000). Treating shock in a timely manner, before hypotension develops, may prevent circulatory collapse.
The two distinct clinical presentations of shock are warm shock (characterized by full, bounding pulses, warm skin, and hypotension) and cold shock (characterized by hypotension and delayed capillary refill). Warm shock is more common in adults, but it is present in only 20% of children who present with septic shock (Zanotti-Cavazzoni and Hollenberg, 2009). Particularly in patients with cold shock, tissue hypoperfusion begins to occur long before compensatory mechanisms fail and hypotension develops (Dabrowski et al., 2000).
Shock resuscitation should begin with assessment of the airway, breathing, and circulation. All children with suspected shock should receive supplemental oxygen. Pulse oximetry is useful, not only to monitor adequacy of oxygenation but also because a poor signal indicative of poor perfusion may prompt a more aggressive resuscitation. Children with shock and severely increased work of breathing, or a Glasgow Coma Scale of less than 8, are at high risk for respiratory arrest, and the airway should be secured. Although etomidate as an induction agent favors hemodynamic stability, it impairs steroidogenesis and has been associated with increased mortality in patients with septic shock (Hildreth et al., 2008; Cuthbertson et al., 2009). Ketamine, because of its favorable effects on hemodynamics and its antiinflammatory properties, may be the drug of choice for intubating patients in shock (Lois and De Kock, 2008).
Vascular access should be established as quickly as possible. Clinicians should have a low threshold for using the intraosseous route. Central venous access is recommended for fluid refractory shock, but resuscitation should begin via intravenous or intraosseous access (Brierley et al., 2009). Anything that can be given through an intravenous line can be given via the intraosseous route. For a child with impaired perfusion, the time to central circulation for drugs administered via the intraosseous route may be shorter than for drugs given though a peripheral intravenous line. A bedside glucose test is appropriate for any acutely ill child, as high metabolic rates and limited glycogen stores predispose infants and small children with sepsis to hypoglycemia. Hypocalcemia is an easily reversible contributor to myocardial dysfunction. An ionized calcium level should be obtained, and hypocalcemia should be treated in the initial phase of resuscitation (Brierley et al., 2009).
Fluid resuscitation should be accomplished as quickly as possible. No consensus exists with regard to the use of crystalloid versus colloid (Brierley et al., 2009). The most common initial resuscitation fluid is normal saline. Crystalloid resuscitation should be delivered in 20 mL/kg aliquots to most patients in 15 minutes or less (Brierley et al., 2009
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree