Indications and Clinical Considerations
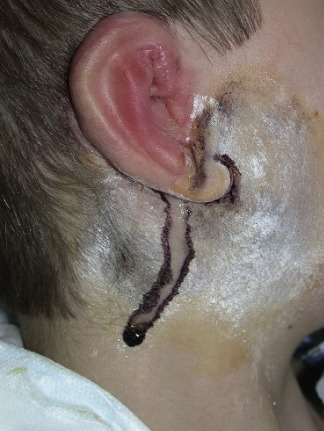
Frey syndrome is a constellation of symptoms including unilateral hyperhidrosis and flushing of the malar region and pinna of the ear that occurs when eating or drinking anything that stimulates the parotid gland to produce saliva ( Figure 13-1 ). Also known as auriculotemporal syndrome, Baillarger syndrome, Dupuy syndrome, salivosudoriparous syndrome, and gustatory sweating syndrome, this disorder usually occurs 2 to 13 months after surgery, open trauma, or infection of the parotid gland. It is thought to be caused by improper regeneration of the sympathetic and parasympathetic nerves subserving the parotid gland and affected anatomic areas. The severity of symptoms associated with Frey syndrome can range from mild to debilitating. Although the incidence of Frey syndrome after parotid surgery can be decreased by careful attention to surgical technique, including careful identification and preservation of the auriculotemporal nerve and creation of a thick skin flap when performing parotidectomy, approximately 5% of patients undergoing parotid surgery will experience some degree of symptomatology. For patients with mild symptoms, reassurance and the use of topical antiperspirants such as 20% aluminum chloride in alcohol or topical scopolamine cream may be all that is required. For more severe symptoms, blockade of the auriculotemporal nerve may provide significant relief. Auriculotemporal nerve block may also be combined with intradermal injection of botulinum toxin A in the areas of hyperhidrosis. Diagnosis of Frey syndrome may be facilitated by performing a Minor starch iodine test, which makes use of Lugol’s reaction to identify areas of sweat production after the patient is asked to suck on a lemon which serves as a sialagogue ( Figure 13-2 ).

Clinically Relevant Anatomy
The auriculotemporal nerve arises from fibers of the mandibular nerve. It courses upward through the parotid gland, passing between the temporomandibular joint and the external auditory meatus, in which it gives off branches that provide sensory innervation to the temporomandibular joint and portions of the pinna of the ear and the external auditory meatus. Ascending over the origin of the zygomatic arch, the auriculotemporal nerve continues upward along with the temporal artery, providing sensory innervation to the temporal region and lateral scalp.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








