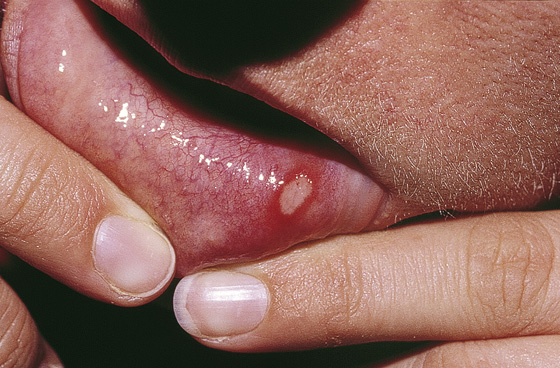
Figure 41-1 Aphthous ulcers. A gray-white oval ulcer with a bright red margin is typical. These lesions are usually quite painful. (From White G, Cox N: Diseases of the skin, 2nd ed 2. St Louis, 2006, Mosby.)
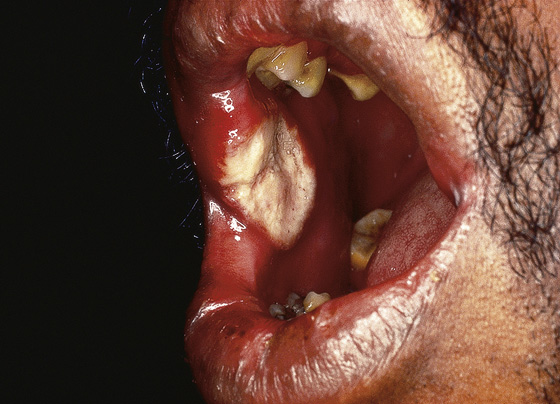
Figure 41-2 Aphthae major in a patient with AIDS. (From Bolognia J, Jorizzo J, Rapini R: Dermatology. St Louis, 2003, Mosby.)
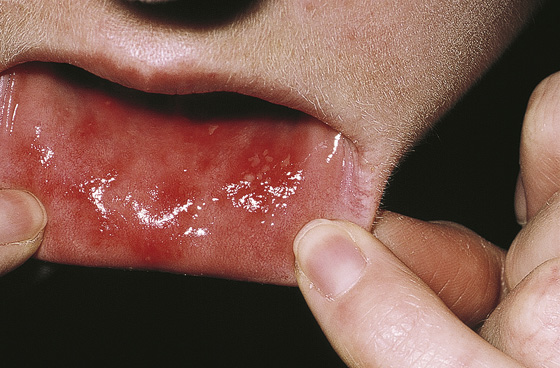
Figure 41-3 Herpetiform mouth ulcers. (From White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
What To Do:
 Through a careful history and physical examination, decide whether the patient is troubled with simple aphthosis or is more likely to have the potentially more serious complex aphthosis.
Through a careful history and physical examination, decide whether the patient is troubled with simple aphthosis or is more likely to have the potentially more serious complex aphthosis.
 Attempt to differentiate between the patient’s mucosal sores and lesions of herpes simplex (most commonly appearing on the lips and skin outside the mouth) (see Chapter 54).
Attempt to differentiate between the patient’s mucosal sores and lesions of herpes simplex (most commonly appearing on the lips and skin outside the mouth) (see Chapter 54).
 For simple aphthosis with minor aphthae, inform the patient that these lesions are benign and usually last 1 to 2 weeks. She should avoid heavily spiced, acidic, or other irritating food and drink, such as pretzels and citrus fruit, and avoid any precipitating factors, such as ill-fitting dentures, a hard-bristled toothbrush, or habitual biting. Avoidance of sodium lauryl sulfate-containing mouthwash and dentifrices (used for foaming action) may decrease the incidence of aphthous ulcers. Interestingly, the antibacterial, anti-inflammatory chemical triclosan has been demonstrated to prevent the chemotoxicity of sodium lauryl sulfate and reduce aphthous ulcers by 96%. Colgate Total (Colgate-Palmolive, New York, N.Y.) is a commercially available dentifrice containing triclosan.
For simple aphthosis with minor aphthae, inform the patient that these lesions are benign and usually last 1 to 2 weeks. She should avoid heavily spiced, acidic, or other irritating food and drink, such as pretzels and citrus fruit, and avoid any precipitating factors, such as ill-fitting dentures, a hard-bristled toothbrush, or habitual biting. Avoidance of sodium lauryl sulfate-containing mouthwash and dentifrices (used for foaming action) may decrease the incidence of aphthous ulcers. Interestingly, the antibacterial, anti-inflammatory chemical triclosan has been demonstrated to prevent the chemotoxicity of sodium lauryl sulfate and reduce aphthous ulcers by 96%. Colgate Total (Colgate-Palmolive, New York, N.Y.) is a commercially available dentifrice containing triclosan.
 If food allergens, such as cereal, fruit, chocolate, nuts, and tomatoes, can be identified as triggering recurrent canker sores, their elimination will reduce or completely relieve symptoms in approximately 90% of cases.
If food allergens, such as cereal, fruit, chocolate, nuts, and tomatoes, can be identified as triggering recurrent canker sores, their elimination will reduce or completely relieve symptoms in approximately 90% of cases.
 Recommend acetaminophen (Tylenol) as an analgesic, adding a narcotic as needed.
Recommend acetaminophen (Tylenol) as an analgesic, adding a narcotic as needed.
 Prescribe Triamcinolone 0.1% in orabase (Kenalog in orabase). Apply a thin film to dried ulcers 2 to 4 times daily until healed.
Prescribe Triamcinolone 0.1% in orabase (Kenalog in orabase). Apply a thin film to dried ulcers 2 to 4 times daily until healed.
 Prescribe amlexanox (Aphthasol oral paste) 5%, 5-g tube, to be applied qid (about 0.5 cm to affected area after brushing teeth). This medication may sting, but it is the first drug to be approved by the U.S. Food and Drug Administration (FDA) for aphthous ulcers in healthy people. This treatment may help canker sores heal only a little faster and could be reserved for those cases in which pain is severe and sores recur frequently.
Prescribe amlexanox (Aphthasol oral paste) 5%, 5-g tube, to be applied qid (about 0.5 cm to affected area after brushing teeth). This medication may sting, but it is the first drug to be approved by the U.S. Food and Drug Administration (FDA) for aphthous ulcers in healthy people. This treatment may help canker sores heal only a little faster and could be reserved for those cases in which pain is severe and sores recur frequently.
 An alternative treatment that can be used for transient pain relief is a tablet of sucralfate crushed in a small amount of warm water and swirled in the mouth or gargled. Another alternative is tetracycline elixir (or a capsule dissolved in water), not swallowed but applied to the lesions to cauterize them or used as a mouthwash. This also stings but sometimes can relieve pain after one or more applications.
An alternative treatment that can be used for transient pain relief is a tablet of sucralfate crushed in a small amount of warm water and swirled in the mouth or gargled. Another alternative is tetracycline elixir (or a capsule dissolved in water), not swallowed but applied to the lesions to cauterize them or used as a mouthwash. This also stings but sometimes can relieve pain after one or more applications.
 Diphenhydramine (Benadryl) elixir mixed 1:1 with kaolin-pectin (Kaopectate), lidocaine (Xylocaine 2% viscous solution), and hydrocortisone (Orabase HCA) applied topically with a cotton-tipped swab can also provide symptomatic relief. Bioadhesive 2-octyl cyanoacrylate (Dermabond) has been recommended as a topical nonprescription treatment for pain reduction but is cost prohibitive if applied repeatedly.
Diphenhydramine (Benadryl) elixir mixed 1:1 with kaolin-pectin (Kaopectate), lidocaine (Xylocaine 2% viscous solution), and hydrocortisone (Orabase HCA) applied topically with a cotton-tipped swab can also provide symptomatic relief. Bioadhesive 2-octyl cyanoacrylate (Dermabond) has been recommended as a topical nonprescription treatment for pain reduction but is cost prohibitive if applied repeatedly.
 For more severe cases, prescribe the topical steroid clobetasol propionate gel (Temovate) 0.05%, 15-g tube. Apply a thin film after drying the area qid until healed. The gel may be mixed with Orabase (OTC) mucosal adherent, although the dilution may affect the strength. Not recommended for patients less 12 years old.
For more severe cases, prescribe the topical steroid clobetasol propionate gel (Temovate) 0.05%, 15-g tube. Apply a thin film after drying the area qid until healed. The gel may be mixed with Orabase (OTC) mucosal adherent, although the dilution may affect the strength. Not recommended for patients less 12 years old.
 In very severe cases, try a burst dose of prednisone, 40 to 60 mg qd for 5 days (no tapering required).
In very severe cases, try a burst dose of prednisone, 40 to 60 mg qd for 5 days (no tapering required).
 Patients with complex aphthosis or with major aphthae can be treated with the same measures as outlined earlier. Approximately 15% of these patients have a systemic disorder in which the oral ulcers are a mucocutaneous marker of the systemic disease. Therefore they should also be referred to a specialist for further evaluation of these possible associated systemic diseases, which may require management with systemic agents to control the aphthae. Such agents include colchicines, thalidomide, dapsone, and cyclosporine. You may also consider vitamin supplementation: zinc lozenges, vitamin C, and vitamin B–complex.
Patients with complex aphthosis or with major aphthae can be treated with the same measures as outlined earlier. Approximately 15% of these patients have a systemic disorder in which the oral ulcers are a mucocutaneous marker of the systemic disease. Therefore they should also be referred to a specialist for further evaluation of these possible associated systemic diseases, which may require management with systemic agents to control the aphthae. Such agents include colchicines, thalidomide, dapsone, and cyclosporine. You may also consider vitamin supplementation: zinc lozenges, vitamin C, and vitamin B–complex.
What Not To Do:
 Do not give steroids to a patient in whom you suspect there may be an underlying herpes infection.
Do not give steroids to a patient in whom you suspect there may be an underlying herpes infection.
 Do not forget to consider hematologic etiologies if recurrent or slow-healing ulcers are associated with fevers. Check a complete blood count (CBC) with differential to rule out neutropenia or leukemias.
Do not forget to consider hematologic etiologies if recurrent or slow-healing ulcers are associated with fevers. Check a complete blood count (CBC) with differential to rule out neutropenia or leukemias.
Discussion
Aphthae is a term of ancient origin referring to ulceration of any mucosal surface.
Aphthous stomatitis has been studied for many years by numerous investigators. Although many exacerbating factors have been identified, the cause as yet remains unknown. Lesions can be precipitated by minor trauma (often from a hard-bristled toothbrush), food allergy, stress, genetic predisposition, allergy, medications, nutritional hematinic deficiencies (e.g., iron, folic acid, vitamin B12), systemic illnesses (e.g., inflammatory bowel disease or gluten-sensitive enteropathy [celiac sprue]), or HIV-associated immunosuppression. Recurrent aphthous ulcers may also accompany malignancy or autoimmune disease.
Behçet syndrome is a multisystem inflammatory disorder characterized by recurrent oral ulcers that are clinically indistinguishable from aphthae but are accompanied by genital ulcers, conjunctivitis, retinitis, iritis, leukocytosis, eosinophilia, and increased erythrocyte sedimentation rate. Patients with posterior uveitis (i.e., retinal vasculitis) are at greatest risk for blindness. Patients with Behçet disease usually present with oral aphthae (minor, major, and herpetiform), which may be the only manifestation of disease for an average of 6 to 7 years before the second major manifestation is apparent.
At present, the treatment for both simple and complex aphthosis is only palliative and may not alter the course of the syndrome. Aphthous ulcers may be an immune reaction to damaged mucosa or altered oral bacteria.
Although they are in great pain, patients with simple aphthosis and minor aphthae can be reassured that they do not have a serious problem and that they are not contagious. Herpangina and hand-foot-and-mouth disease can produce ulcers resembling aphthous ulcers, but these ulcers are instead part of Coxsackie viral exanthems, usually occurring with fever and in clusters among children.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


