Oxygen tubing via nasopharyngeal airway technique.
Blood pressure is closely monitored and although lower pressure is desirable to decrease the risk of hematoma formation, caution should be exercised in the older patient population with long-standing hypertension as they are prone to cerebral ischemia. Infrared brain oxygen monitor with pads on the forehead may be an expensive but useful option in high-risk patients. Cases of carotid stenosis should be identified and carefully managed. This concern should be discussed with the surgeon and the lowest blood pressure safe for a particular patient should be agreed upon by both anesthesiologist and surgeon. A sudden increase in blood pressure due to epinephrine absorption can occur. Care should be taken not to manage this with beta-blockers alone as this can give rise to unopposed alpha stimulation, which can lead to severe vasoconstriction in the face of cardiac beta-blockade, resulting in pulmonary edema. If intravascular injection is suspected, the surgeon should be informed immediately. Although surgeons prefer blood pressure to be on the lower side, some of them may request normotensive pressures before flap closure to ensure sufficient hemostasis. Temperature monitoring and maintenance of normothermia, especially in longer cases, not only ensures patient comfort but helps to decrease negative patient consequences. These include bleeding, which can lead to hematoma formation, surgical site infection, morbid cardiac events, and prolongation of post-anesthesia discharge time to home.
The maintenance of general anesthetic can be achieved with either inhalational or intravenous agents in intubated patients. Emergence is usually smoother in intubated patients receiving total intravenous anesthesia. In our practice, propofol is nearly always used in conjunction with another medication in subhypnotic doses for this purpose. Ketamine is one of the adjuncts and can be added to propofol in concentrations ranging from 0.25 to 1.5 mg/ml, titrated to patient requirements of sedation or general anesthesia.[21] However, it should be remembered that ketamine causes increased salivation that can lead to coughing and laryngospasm in an unintubated patient. The lower dose range is not associated with postoperative nausea and vomiting or delayed discharge. Another drug combination that has been used successfully is alfentanil and propofol, both for general anesthesia and mild to moderate sedation. Alfentanil is infused over a dose range of 0.2–0.4 µg/kg/min and propofol 25–75 µg/kg/min.[22] It has a faster onset than fentanyl but a shorter duration of action. During deep sedation, it has been shown to cause oxygen desaturation. Remifentanil infusion can also be safely titrated in spontaneously breathing unintubated patients and in intubated patients. It has been shown that the risk of postoperative hypertension is increased after remifentanil-based anesthesia. The underlying mechanism, although not completely understood, has been attributed to abrupt cessation of analgesia or acute opioid tolerance.[23,24] This may be a concern after facelift where there is a risk of hematoma formation, especially in the setting of ongoing absorption of previously infiltrated epinephrine. Blood pressure should be closely monitored and managed accordingly. Anti-emetic prophylaxis is extremely important is plastic surgical procedures as straining during retching and vomiting can also increase blood pressure.
Post-anesthesia recovery room (PACU)
The key points of anesthetic care, including but not limited to blood pressure management, normothermia, and anti-emetic management, should be continued in PACU, too. PACU staff should be directed to watch for any sign of hematoma formation and respiratory distress. In the rare situation of airway obstruction, the wound may have to be opened immediately. Timely diagnosis and evacuation of hematoma not only averts respiratory emergency but also leads to normal healing. An emergency plan should be in place for surgical evacuation of hematoma.[7] Anesthesiologist and operating room nursing personnel should be available until the decision is made to discharge the patient. Equipment to emergently secure the airway should be at hand, operating room set up before staff leaves, and a sterile set of instruments available. Evacuation of hematoma may require intravenous sedation or general anesthesia depending upon the situation and anxiety level of the patient.
Tumescent anesthesia for liposuction
Liposuction is one of the most common ambulatory cosmetic procedures performed in the United States, and tumescent anesthesia is widely used for this purpose. Surprisingly, there is a dearth of articles or any comprehensive guidelines on this topic in anesthesia literature in spite of many of us being involved in the perioperative management of these cases.
Tumescent anesthesia is regional local anesthesia of the skin and subcutaneous tissue. This technique was first described by a dermatologist, Dr. Jeffry Klein.[25] It involves the ballooning of subcutaneous fat with large volumes of dilute lidocaine and epinephrine solution in normal saline or Ringer’s Lactate. The concentration of lidocaine ranges from 0.025% to 0.1% as compared to the traditional 0.5–2% used for nerve blocks or field blocks. One milligram of epinephrine is added to each liter of solution with resultant final strength of 1:1,000,000 (1 µg/ml). Approximately 3–4 ml of the infiltrate is infused for each planned milliliter of aspirate. Subcutaneous infiltration of large volumes of this solution produces swelling and firmness (tumescence) of tissues. Fat is detached from the subcutaneous skin with the help of liposuction cannulas and up to several liters of emulsified fat are suctioned or aspirated. Aspiration can be either manual or power-assisted.
The major dichotomy that is faced by anesthesiologists is the dose of lidocaine used for tumescent anesthesia. According to Practice Advisory on Liposuction,[26] “it is generally accepted that a lidocaine dose of up to 35 mg/kg is safe when injected into the subcutaneous fat with solutions containing epinephrine, although doses up to 50 mg/kg have been utilized.” This goes against our training of a conventional maximum allowable dose of 7 mg/kg. This dose, when used as 1–2% lidocaine for neuraxial blocks, nerve blocks, and skin infiltration, is constrained by the development of central nervous system toxicity. In comparison, tumescent anesthesia doses have been used in tens of thousands of procedures with minimal harm. This duality of lidocaine dosing has been attributed to the fact that a very dilute solution (1 mg/ml) is slowly infiltrated into a poorly vascularized space. Because liodcaine is relatively lipophilic, it binds to the extensive shallow subdermal fat reservoir in the range of 1 mg of lidocaine per gram of tissue, and some of this is removed when the lipid is aspirated out. This large absorption buffer retains lidocaine in comparison to concentrated (10 mg/ml or 1%) lidocaine, where 1/10 mg is absorbed by the buffer and 9/10 mg remains unbound and can be absorbed in systemic circulation, leading to elevated levels in blood.[27] Epinephrine in the solution has a vasoconstrictive effect that also slows and decreases the systemic absorption of lidocaine, resulting in lower peak blood levels and increased duration of analgesia.[28] It has been shown that after 1% lidocaine injection for epidural block and intercostal nerve block, peak blood levels are achieved in approximately 7 and 8 minutes, respectively.[29] In contrast, lidocaine peaks 8–16 hours after infiltration for tumescent anesthesia.[28]
In addition to difference in peak effect, there is a difference in clearance of lidocaine from systemic circulation, too. Two hours after epidural lidocaine injection, lidocaine blood level is negligible. Measurable levels of lidocaine and its metabolite persist for more than 36 hours after tumescent anesthesia.[27]
Although tumescent doses of lidocaine have been used safely, neurologic and cardiac toxicity can occur due to various reasons. Lidocaine is metabolized in the liver by the CYP 450 enzyme family and toxicity depends on the ratio of its absorption and removal from the blood. Any limit on hepatic clearance can prolong lidocaine persistence in the circulation, resulting in serious toxicity. Various drugs can cause competitive inhibition of the CYP 450 system. Some of these drugs that are commonly used are alprazolam, carbamazepine, erythromycin, losartan, and simvastatin. As hepatic lidocaine clearance is flow-dependent (rather than substrate-dependent), enzyme saturation is a bigger concern than competitive inhibition. This means that a massive lidocaine load can overwhelm the CYP 450. Toxicity from tumescent lidocaine can initially present as cardiac toxicity instead of CNS symptoms as slow rise and prolonged elevated levels progressively depress cardiac conduction and contraction, ultimately leading to circulatory failure. Careful calculation of maximum tumescent lidocaine dose is essential to minimize the risk of toxicity. It is also important not to combine tumescent anesthesia with procedures requiring regular-strength lidocaine (nerve blocks or local infiltration for various procedures).
Volume overload is another important risk associated with tumescent anesthesia. As previously mentioned, a substantial volume of anesthetic solution (3–4 ml infiltrate/ml of planned aspirate) is injected to produce tumescence. This can add up to 800–2000 ml for abdomen, 400–1000 ml for each hip, 500–1200 ml for each lateral thigh, and same volume for each medial and anterior thigh, respectively. Fifty to seventy percent of infiltrate is left behind at completion of procedure and gets absorbed.[26] Fluid overload can result in serious complications such as pulmonary edema and electrolyte imbalance. Communication with the surgeon on fluid management is critical and it is imperative to monitor fluid input and output throughout the case and afterwards. At completion of the procedure, calculation of residual volume helps to determine postoperative care. If large volume liposuction (> 5000 cc of aspirate) is planned, it should be performed as inpatient instead of ambulatory procedure. Patients should be monitored overnight for stability of vital signs and urine output. Large-volume procedures should be done as separate serial procedures.[26]
Intraoperative hypothermia can be another consequence of large-volume tumescent anesthesia and appropriate measures should be taken to prevent and manage it, such as using pre-warmed (37°C) fluid.
Like any other surgical procedure, serious consideration should be given to prophylaxis for deep vein thrombosis which can result in pulmonary embolism. There have been reports of death from fat emboli, too.[26] Fat emboli can occur from both mechanical (absorption of fat globules) and biochemical reasons (inflammation from circulating fatty acids causing damage to pneumocytes).
The choice of anesthesia for tumescent liposuction depends on patient status, site and extent of the procedure, and the patient’s level of comfort. Complex procedures are better done under general anesthesia to provide a motionless surgical field and airway control. Liposuction over the abdominal wall is relatively high-risk due to the repetitive motion of the trocar in close proximity to critical viscera such as the liver (Figure 12.2). Any sudden patient movement or coughing can cause hepatic injury so adequate depth of anesthesia is imperative. Epidural and spinal anesthesia in the ambulatory setting might not be suitable for large-area liposuction as sympathectomy from neuraxial anesthesia can lead to vasodilatation and hypotension which is usually managed with intravenous fluid infusion. In this particular situation where the patient is already receiving tumescence fluids, this can increase the risk of fluid overload.
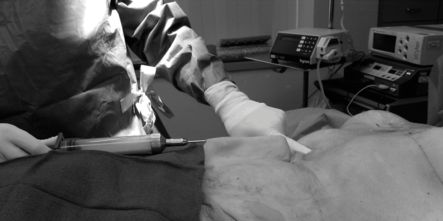
Liposuction trocar in close proximity to liver.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




