(1)
Northern Anesthesia & Pain Medicine, LLC, Eagle River, Alaska, USA
(2)
WWAMI Program, University of Washington School of Medicine, Anchorage, Alaska, USA
Keywords
OpioidHostDependenceAddictionPseudoaddictionCravingChoiceCompulsionConditioningOperantIncentive sensitizationRewardHedonic toneOpponent processAllostasisLocus of controlBiologic modelDisease modelDopamineMesolimbicStriatumNucleus accumbensVentral tegmental areaOrbitofrontal cortexLateral prefrontal cortexDRD2 receptorΔFosBEpigeneticPreventionSpiritualPeer supportPRIME theoryMotivationA 26-year-old male presents to your practice with a complaint of low back pain that he states has been troubling him for 8 years and which he attributes to manual labor as a roofer and also a history of multiple motor vehicle accidents. There are no radicular nor cauda equina symptoms . He states that physical therapy has failed to benefit him as have NSAIDs and tramadol. He reports that he has been using hydrocodone-acetaminophen products for the past 5 years, currently using eight 10/325 tablets daily and that this is the only therapy that “works for him” and allows him to remain functional as a roofer. He is a smoker and admits to two to three beers per evening. Upon further questioning he admits to regular use of marijuana as well. Family history is remarkable for a “bad back” in his father, who underwent several spine operations in his 40s and 50s. Review of systems is positive for insomnia and constipation. Review of the PDMP shows multiple hydrocodone prescriptions by various providers, mostly emergency room physicians, filled at various pharmacies.
On exam he is well-developed, well-nourished, alert, and oriented x4. Vital signs are T99.5, HR 108, BP 166/98, RR 18. Pupils are 8 mm. There are no fresh punctate wounds nor tracks, and he exhibits no stereotypic stimulant behaviors. He is without any obvious neurologic deficits. His lumbar spine ROM is limited in flexion and extension by pain, and there is obvious thoracolumbar myospasm. Straight leg raise is negative bilaterally, as are Kemp’s and Patrick’s maneuvers.
He requests that you prescribe him “240 ‘hydros’ for the month.”
Introduction
We turn our analysis now to the final component of the classic epidemiologic triangle, and that which is arguably the most complex, as well as the most important: the host. In the arena of infectious disease epidemiology and public health efforts, attempts to intervene upon the agent itself are generally of very limited utility; similarly, while alteration of opioid agents (the subject of Chap. 5) has shifted abuse patterns, we have not seen concomitant decrease in consumption, misuse/abuse, or adverse consequences. Vector modification (e.g., reduction of mosquito populations) has borne some success in certain disease reduction efforts; similarly, modification of prescriber practices may be fruitful by certain metrics (e.g., reduced methadone overdose). The overall data however are not as encouraging; opioid death rates increased by 15.6% from 2014 to 2015 and surpassed 33,000 deaths in 2015 [1]. While “street drugs” (heroin and illicitly manufactured fentanyl) were responsible for most of the increase, abuse of prescription opioids has not declined significantly (with possible increase over the past year) and furthermore continues to elicit concern as a “gateway” to heroin, etc. (Fig. 9.1).
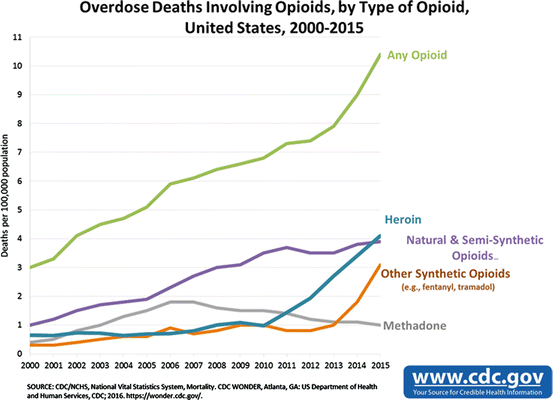

Fig. 9.1
US opioid deaths , 2000–2015. Source: CDC/NCHS, National Vital Statistics System, Mortality. CDC WONDER, Atlanta, GA: US Department of Health and Human Services, CDC; 2016. https://wonder.cdc.gov
Regardless of the source and structure of the opioid involved, it is clear that efforts to date (e.g., nearly $29 billion federal monies spent in 2015, with $31 billion earmarked in 2017 [2]) have not yet been sufficient to turn the tide.
It is the author’s contention that, as with other historically significant epidemics, success in reversing the grim and rising toll of opioid morbidity and mortality will come only with alteration of host factors including vulnerability and exposure behaviors. Despite modern-era elucidation of agent factors (e.g., mutations in influenza strains rendering them exponentially more capable of ravaging vulnerable populations) as key determinants of infectious organism pathogenicity/virulence , current evidence suggests that exclusive focus on the agent is antiquated and reductionist. Our understanding of the complex interactions between host and agent has grown to include an appreciation for the commensal if not even symbiotic relationship between many microorganisms and human beings, and diminution of host resistance is known to be a key element in the balance between health and disease.
In the area of opioid misuse and abuse, host vulnerability to the agent rather than agent virulence may represent the more important area of focus given that we remain largely reliant upon (appropriate) therapeutic opioid use for the control of much severe and acute pain. Dr. Sydenham’s recently often-quoted applause of opiates:
remains admissible today. Until safer means analgesic means of similar potency (and broad spectrum) become widely available, the judicious application of mu-agonists remains inevitable for the effective treatment of acute pain. As such, adaptation of the host to enable containment and control of the agent is of the essence (Fig. 9.2).
And here I cannot but break out in praise of the great God, the Giver of all good things, who hath granted to the human race, as a comfort in their afflictions, no medicine of the value of opium, either in regard to the number of diseases that it can control, or its efficiency in extirpating them. [3]

Fig. 9.2
Epidemiologic triangle
The propagation of an infectious epidemic is retarded when exposure of vulnerable hosts to the agent falls below a certain threshold rate, and the epidemic itself is eliminated with the eventual development of resistance or immunity within the population. Historically the pressures of natural selection within these dynamics have been the sole mediator of adaptation and survival; more recently within human history, we have been able to engineer immunity with vaccinations, etc. While immunity in the form of long-term mu-opioid receptor blockade by depot naltrexone (or occupancy by buprenorphine) is currently state-of-the-art prevention, the development of a literal “vaccine” for opioids has been contemplated and even explored [4]. Such measures however are not without their disadvantages, as might be expected from disruption of natural processes with the complexity/ubiquity of the endogenous opioid system. One of the more immediate and obvious consequences of such a strategy, well known now to trauma and perioperative practitioners is the marked difficulty conferred by such pharmacologic constraints upon acute pain control. Furthermore, as suggested by the apparent trend away from prescription opioids to heroin attributed to agent/vector modification, restriction of mu-agonist efficacy may only serve to drive a shift in “drug of choice” away from opioids to other substances capable of eliciting similar reward-seeking behavior.
Cultivating control and containment over perceived “appropriate requirement” for opioid analgesia, i.e., pain, (and certainly over inappropriate euphoric or other mood-affecting properties) is critical to overcoming dependence and addiction individually and arguably at a societal level as well. This effort is arguably also the most salient (and collectively overlooked) province toward which medical and public health endeavor should be directed. As discussed in Chap. 1, a critical and assumed ingredient in a population’s effort to end an epidemic is the inherent desire of the vulnerable population to avoid the agent. Unfortunately in the case of addiction, rational self-preservation instincts are surrendered or are conquered by the overwhelming compulsion to seek the addictive substance (or activity) regardless of the results. What renders some hosts more vulnerable than others to such compulsion for inappropriate or even uncontrolled use is a key question, explored in greater detail in Chap. 10.
Outcome Definitions
The attention of the nation, and that of policymakers both governmental and professional, has been upon overdoses. Defining outcome variables is of course important in any scientific analysis, and failure to clearly delineate such renders investigation and conclusions empirical. Quantifiable metrics such as emergency room overdose visits and deaths attributable to opioids provide some means of attempting to track the efficacy of interventions, but comprise only the tip of the proverbial iceberg. While overdoses certainly occur in the opioid-naïve, underlying these outcomes is a much more prevalent problem of opioid dependence and addiction that is not only driving mortality figures but also confers tremendous morbidity physically, psychologically, spiritually, relationally, and societally.
There are significant difficulties involved in attempting to investigate dependence and addiction. Descriptive statistics, let alone analyses are hampered by the challenges of a broad spectrum of “subclinical” illness , lack of criteria consensus, and insensitive instruments for identifying the conditions, to name a few.
As discussed in Chap. 3, by most commonly accepted definitions, the state described as opioid dependence involves recurrent use, withdrawal phenomena, and behavioral components including desire/unsuccessful attempts to quit, effort expended in pursuit of opioids, etc. Addiction is a term currently again deliberately avoided by the American Psychiatric Association (and the World Health Organization) yet commonly used in the scientific community (e.g., NIDA) to describe “compulsive drug seeking despite negative consequences.” As discussed previously, the trend is currently away from the attempted specificity of categorical variables and toward the sensitivity of a continuum, and the DSM-5 has recently described a spectrum of opioid use disorder (OUD) that “includes signs and symptoms that reflect compulsive, prolonged self-administration of opioid substances that are used for no legitimate medical purpose or, if another medical condition is present that requires opioid treatment, that are used in doses greatly in excess of the amount needed for that medical condition” [5]. Four main “symptom clusters” within the current substance use disorder framework include impaired control, risky use, social problems, and physical effects such as tolerance and withdrawal.
Pseudoaddiction is a concept/term not considered previously in this book, which was originally coined in 1989 [6] and gathered some support within the pain management community while failing to gain recognition and acceptance by the greater medical and psychiatric communities. The concept proposes in essence that inadequately treated pain can cause individuals to escalate pain behaviors in order to acquire more opioids. The only real distinction between pseudoaddiction and true addiction in this paradigm is whether the patient cites pain or euphoria-seeking as the reason for opioid-seeking and whether they correspondingly attribute cessation of aberrant drug-related behaviors and opioid misuse after subjective report of pain relief. The difficulties in this theoretical construct (including lack of any scientific basis, plentiful pharmacologic industry support for the reports) have been objectively criticized in recent publications [7–9].
Common to this continuum (dependence, “pseudoaddiction,” addiction) is the disordered behavioral state the American Psychiatric Association describes as “compulsive, prolonged self-administration.” Whether the primary underlying motivation is a relief from physical or mental suffering or merely pleasure-seeking, failure to exercise control over powerful impulses and desires characterizes OUD. Regardless of the outcome variable chosen, at the heart of the opioid epidemic lies loss of control. This final section of the book is concerned with preventing that loss of control or reinstating lost control to the habituated user. While addictionology comprises a very small part if any of the most clinicians’ practices, growing appreciation of the hitherto unrecognized prevalence (and incidence) of substance use disorders should motivate physicians in all fields to, at the very least, familiarize themselves with the basic issues at hand, especially in the era of heavy-handed pharmacotherapy. Certain fields more than others share overlap with the domain of addictionology and also carry increased liability for iatrogenic facilitation of addiction. It is assumed that the self-selected audience of this book falls within this latter category, and as such, this entire chapter is devoted to presenting a hopefully comprehensive yet concise clinical framework of addiction theory.
Overview of Addiction
West and Brown [10] define addiction as “a chronic condition in which there is a repeated powerful motivation to engage in a rewarding behavior, acquired as a result of engaging in that behavior, that has significant potential for unintended harm.” This elegant definition has shed some of the conventional thought and language concerning addiction (e.g., unsuccessful desire to disengage from the behavior, which may or may not be present; use despite significant harm and loss, which may or may not occur) and as such is more applicable to the spectrum of OUD that has traditionally fallen outside that rubric. As mentioned above, we will use the language of addictionology within the brief survey presented below to encompass this expanded scope and hopefully inform better care across the spectrum of severity. At the outset of this discussion, we will present some commonly observed cardinal features/characteristics of addiction pertinent to both preventive and therapeutic efforts, followed by some basic clinical and public health questions framed around these and related phenomena.
Finally, a survey of addiction theories and models is presented. Most of these theories and models generally exhibit fairly unidimensional foci (e.g., moral failure, genetic predisposition, dysregulation of mesolimbic dopaminergic activity, social learning). While many do not lend themselves well to a systematic organization, in general they have historically been categorized into moral/spiritual, disease, and learning models. At the heart of the controversies about addiction lies the issue of control, and the (possibly oversimplistic) question of whether choice or compulsion drives the initiation and perpetuation of these behaviors; the complexities of human behavior and the very definition of “choice” (or compulsion) itself render it unlikely that a clear-cut answer will ever be arrived at. There is a growing sense that both may be true, just as light is both particle and wave.
In this chapter we will follow the general outline of models based on choice vs. compulsion and attempt to frame major theories within the context of these two opposing viewpoints as applicable. Integrated into the section on condition/learning is a brief discussion of the observation that addiction generally follows a biphasic course of positive reinforcement/reward followed by negative reinforcement (withdrawal phenomena) which to many forms a bridge or transition between the bipolar constructs of choice vs. compulsion. More recently, social and system models have been proposed and are briefly introduced as well, as they are certainly germane to public health if not individual prevention efforts. The chapter concludes with consideration of the complex phenomenon of motivation as a critical consideration in the analysis and prevention/treatment of OUD.
Cardinal Phenomena of Addiction and Related Questions
To date, there has never been a reported case of congenital addiction . Whether or not the condition is heritable or latent may be debated until the end of time, but it is clear that an initial exposure initiates the process. While outliers of truly forcible exposure (not mere “peer pressure”) undoubtedly exist, for the most part this introduction to the substance follows a conscious decision, often facilitated by some perceived well-being deficit, whether pain, emotional distress, or simply boredom. Not everyone exposed, however, whether once or repetitively, goes on to develop dependence and addiction. Despite multiple substances with addictive potential, people furthermore generally seek out and develop a dependence upon a “drug of choice” or a limited combination thereof (e.g., alcohol and tobacco, or opioids and benzodiazepines).
In those in whom addiction develops, a well-documented progression from a “positive” reward-chasing cycle to one of “negative” pursuit of the habituated substance to avoid withdrawal phenomena exists. During the initial reward-mediated phase , powerful cravings for the substance generally develop that are inversely proportional to an inevitable experience of diminishing returns. This satisfaction-resistant drive supersedes/subjugates all others, and the pursuit of the substance becomes singular at the expense of all other goals and priorities. Ultimately (sometimes within a very short period) the switch to negative reinforcement occurs, mediated by powerful withdrawal symptoms both psychological and physical, and avoidance of this discomfort becomes the primary motivating factor. More often than not, the individual struggles with this increasing captivity and makes efforts to resist and desist to some degree. Relapse after varying periods of sobriety is common.
Questions to consider include:
What makes some people more prone than others to develop addiction?
Why do youth appear to be disproportionately vulnerable?
What are the psychological processes (and risk factors) involved in the development and maintenance of addiction?
What are the neurobiological processes (and risk factors) involved in the development and maintenance of addiction?
What are the social processes (and risk factors) involved in the development and maintenance of addiction?
How much overlap is there between choice and compulsion in the development and maintenance of addiction?
How much common ground do the many apparent distinct “pathways to addiction” including different initial motivations, different substances, different biochemical/genetic profiles, etc. share?
Are we doing enough to educate individual patients or the populace as a whole about the manifold dangers of addiction?
What motivates people to succumb to addictive behavior?
How do we help confer resistance/immunity to addiction?
How do we best intervene when addiction has developed? Is there a single best approach or multiple options best tailored to individual situations?
Addiction Theories and Models: Choice
The viewpoint of addiction in the West was dominated by choice models up until the latter part of the twentieth century. Until modern era tobacco-related mortality (coupled with its ubiquity—there are 33 million daily American tobacco users in 2014 vs. 16 million “heavy” alcohol users [11]) commandeered public health attention and monies, alcoholism has historically served as the prototypical and most studied addiction. Excessive use of alcohol has been viewed as aberrant since antiquity, with recognition of adverse physical health consequences as well as relational and societal damage documented for millennia in the Hebrew Scriptures and other sacred texts. The prevalent spiritual/religious influence on human behavior in most pre-industrial societies was generally associated with a viewpoint on behavioral excesses in general as immoral and deliberately defiant of a Divinely prescribed order. Inherent in that transgression is the concept of choice.
Choice in common parlance involves an independent decision free of predetermination or constraint. It exemplifies the concept of free will and an internal locus of control. Choice is not necessarily at odds with habituation nor indeed with vulnerability nor predisposition to certain behavioral patterns. It does not imply rational/logical thought nor self-interest.
The determination of whether decisions or behaviors are rational or irrational depends of course upon the definition of those terms and concepts. Closely linked with this evaluation is whether the party rendering such judgment appeals to an external comparison standard of good/best/right and whether that comparison standard is absolute or relative. Relevant questions include:
Does rational choice require full comprehension of risks, benefits, and alternatives?
How can such comprehension be determined/does simple verbal assent really signify understanding?
Is the standard the highest good of the individual or that of their local or larger society?
Does highest good mean absolute absence of negative/harmful actions or the “best we can do/lesser of two evils” in terms of balancing competing benefits and harms?
Does highest good entail conformity/compliance with an external code of behavior?
Some thought leaders (and certainly a multitude of individual users) take the position that substance abuse and dependence/addiction may in certain situations be adaptive rather than maladaptive. Addiction models mirroring this stance propose that underlying the behavior lies a rational choice to escape from/self-medicate physical or emotional pain, stress and anxiety, concentration/resolve difficulties, angst, or simple boredom. Again, such calculated decisions do not necessarily reflect a fully informed position nor one accurately weighing the relative cost of future consequences against current perceived needs. The etymologic origin of the word rational however stems from the Latin ratio, involving a reckoning/calculating, and thus to be true to the language, any decision weighing pros and cons is technically rational, regardless of the scope of information considered or the degree of foresight involved.
The traditional (and general current consensus) viewpoint however is that the unregulated behavior of addiction in general, and in the context of this book, opioid use disorder specifically is irrational. Individual adverse effects abound as discussed in Chap. 3, and addiction almost universally results in harm to the addict’s wider psychosocial context as well, including strained family and societal relationships, loss of productivity, and criminal issues. Most consensus definitions of addiction have invariably included compromise of these arenas; the current DSM-5 substance use disorder social impairment category [5] includes:
Among its criteria, all are generally deemed irrational by both professional and lay communities. In Dr. Jim Orford’s words, addiction “spoils many lives, and often shortens them” [12].
Repeatedly unable to carry out major obligations at work, school, or home due to substance use
Continued use despite persistent or recurring social or interpersonal problems caused or made worse by substance use
Stopping or reducing important social, occupational, or recreational activities due to substance use
Choice models recognize a continuum of impaired decision-making generally beginning with initial experimentation and frequent underestimation of the addictive potential of the substance in question. At this stage, prior to the development of habit or compulsion, regardless of the latitude of behavioral and biologic philosophy, it is patently difficult to attribute use to anything but choice.
During the reward-seeking phase of addiction, in which ongoing and generally increasing use is reinforced by “positive” but diminishing effect, it is similarly difficult to refute the element of choice without essentially denying the human capacity/function of the will, despite the presence of potentially overwhelming desire and craving. Craving may be simply a matter of unregulated, “excessive appetite” [12] although it is, as alluded to above, an “acquired taste” reinforced by psychological conditioning and neural adaptation [13]. During this period there is a transition from “unstable preferences” [14] in competition with each other to solidification of purpose with ascension of the addictive pursuit to supremacy. The degree to which conflicting desires and ideology exert opposition is as unique as each individual and is based on varying levels of information, worldview and conviction, relevance and potency of competing motives (in many cases “I’ve got too much to lose” is sufficient disincentive), etc. Numerous neurobiological processes and adaptations are at work during this period as well, as discussed in greater detail later. Regardless of the relative inputs and interface between the biologic/physical and the psychologic/metaphysical, decision-making and choice play a paramount role in indulgence vs. abstinence and in the progression vs. abatement of addiction.
Addiction as Learned Behavior
There is no doubt that conditioning forms an essential part of the addictive process. There is much disagreement (as with most aspects of addiction) as to whether such learning/behavioral habituation represents compulsion or choice. While many regard conditioning as an ever-increasing state of helplessness, it clearly involves reinforcement of volitional behaviors and as such these models are considered under the rubric of addiction as choice in this survey.
Reinforcement of behavior is generally considered to occur as a result of direct pairing of a stimulus with a positive or negative response in the memory of the learner. This instrumental or operant conditioning is at the heart of habit formation and transcends the conscious/unconscious barrier, as evidenced by people lighting up a cigarette without even realizing it. Classical (Pavlovian) conditioning, whereby a secondary stimulus (e.g., Pavlov’s bell or a particular setting) becomes associated with the primary stimulus (e.g., meat or drug use), is well known to scientists, clinicians, and lay counselors alike to play a powerful role in addiction development and maintenance. These cues (e.g., “people, places, things” in the Alcoholics Anonymous lingo) often generally operate at the level of the subconscious and may well develop greater motivational power than the substance itself, especially as tolerance to the substance builds. The incentive sensitization theory formulated by Robinson and Berridge [15, 16] recognizes a distinction between wanting the substance vs. liking it, especially as time progresses and the reward diminishes, yet desire increases. This increasing “incentive salience” is postulated as underlying the overpowering cravings for the substance that develop despite waning positive reinforcement.
The well-known and consistent phenomenon of progression from a positive reinforcement-/reward-driven state to one of negative reinforcement avoidance involves “macro-level” psychobiological adaptations that presumably occur in concert with “micro-level” conditioning . Neurobiological correlates (and their ever-evolving nature) thought to be associated with this transition are discussed below; from a broader theoretical perspective, the opponent process theory of Solomon and Corbit [17] has been widely adapted to the field of addictionology. In general this theory proposes that highly pleasurable (or unpleasant) experiences generate an antagonistic or opponent response to restore emotional homeostasis; over time, desensitization to the initial stimulus occurs while the strength and duration of the opposing force appears to increase. In the context of addiction, tolerance and/or other mechanisms reduce the positive reinforcement; however, both physical and psychological withdrawal (opponent processes) gain increasing motivational power. Koob and Le Moal added to this general framework with their allostatic theory, postulating that a “chronic deviation of reward threshold” [18] occurs as a result of both decrease in reward sensitivity with repeated exposure and an augmented reactionary hormonal stress response. This altered hedonic threshold drives further drug-seeking not so much to achieve pleasure any longer but rather in an attempt to return to baseline.
Addiction as a Spiritual/Religious Problem
Spiritual/religious models for the most part fall under the (irrational) choice rubric as well. Inherently irrational deviation from an absolute (or even relative) standard of good/right behavior defines this perspective. It is an overly simplistic and ill-informed criticism of spiritual/religious models however to characterize them across the board as pure choice models prescribing improved willpower as the solution to overcoming addictive or other maladaptive behaviors. The widely acclaimed 12-step model introduced by Alcoholics Anonymous in the 1930s begins with the famous “I have a problem” confession (We admitted we were powerless over alcohol—that our lives had become unmanageable [19]) and is much more congruent (as is the quote from St. Paul gracing the Part heading) with an understanding of solidified behavior patterns that have escaped the control of the individual. “Voluntary slavery ” as described by Welch [20] describes a potency of compulsion at least equal to that of any biologic model and furthermore carries a more broad theoretical construct invoking the possibility of external control hearkening back to Martin Luther [21], St. Augustine [22], and holy writings centuries older than that.
The defining characteristic of spiritual/religious models is a deviation from right, not just choice. Many of these models recognize (and have helped draw attention to) the progressive loss of control. Key foci also include values and motivation (increasing in popularity both within addiction theory as well as therapeutic approaches). Addiction is often conceptualized in terms of a suboptimal attempt to meet valid needs/fill a void and in some paradigms even an aberrant form of worship [20, 23].
Addiction Theories and Models: Compulsion
As with choice, what comprises compulsion is hazy and fluid. Collins Dictionary of Law [24] defines compulsion as “the forcible inducement to act.” In the legal arena, this generally indicates that significant threat to the individual’s life or well-being is under exercise by an external source. Such extremis, of course, rarely applies to the realm of psychology and behavioral disorders, and Oxford’s “softer” definition [25]—“an irresistible urge to behave in a certain way, especially against one’s conscious wishes”—encompasses reasonable pressures exerted upon the psyche by internal forces (not exclusive of external influence).
The underlying thesis of compulsion models is that powerful psychobiological forces drive the addicted (and in some models, even the naïve but genetically predisposed) individual to engage in repetitive and uncontrolled behaviors over which they have lost control, if ever they possessed it.
Introduction to Biologic/Disease Models
The current addictionology landscape is dominated by the viewpoint that addiction is a medical illness caused (or at least explainable) by perturbations of normal cerebral function. While not equivalent concepts, these terms “disease model” and “biologic model” are used jointly/interchangeably throughout this book to refer to the evolving concept that addiction is the result of functional or even structural abnormalities within the brain. Observations regarding the similarity of alcoholism to other known disease states began to find expression in the nineteenth century [26–28], but it was not until the American Medical Association’s House of Delegates in 1956 first declared alcoholism an “illness” [29] (subsequently labeling it a “disease” in 1966) that the door opened to a gradual and widespread reconceptualization of addiction among the medical and scientific communities. Supporters of this viewpoint drew attention to the fact that alcoholism exhibits a well-defined pattern of symptoms (and sequelae), with a generally chronic and progressive course, and may be treatable although shows significant vulnerability to relapse. The most notorious proponent of the alcoholism-as-disease theory was E.M. Jellinek, whose landmark treatise “The Disease Concept of Alcoholism” [30] in 1960 is still widely credited with bringing this theory into its current place of prominence. Jellinek’s work and even credentials however have fallen into disrepute lately as it appears that much of both were fabricated, and there are allegations that much of his published data were heavily biased and influenced by third party agendas [31–34].
Regardless of the veracity or reliability of Jellinek’s work and construct, the disease model’s ascension to prominence has facilitated considerable scientific and medical research, shedding light on neurobiologic substrates and genetic expressions that appear to be associated with increased addictive behaviors.
Genetic Models
Some of the earliest evidence suggesting a biologic basis for addiction arose from observations that predisposition (and in extreme cases predetermination) to addiction is heritable. Clustering of behavior patterns within families and apparent preservation of the association despite early overhaul of the environment, e.g., adoption of the offspring by non-addicted parents, led to the hypothesis of a genetic vulnerability to addiction.
The explosive advances in DNA sequencing technology over the past three decades have facilitated the identification of numerous genes associated with substance use disorders and dependence/addiction including the well-studied DAT1 gene (encoding the dopamine transporter), polymorphisms of which have been linked to numerous pathologic states involving dopaminergism including conditions as diverse as alcoholism, Parkinson’s disease, and schizophrenia [35]. Several other allelic variants encoding various dopamine receptor and metabolic function including the ANKK1 gene TaqIA1 variant [LAWF1, MOY1], the DRD2 gene rs6277 variant [36], and the DBH gene rs1611115 variant [37] have all been associated with opioid and other substance use disorders.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








