CASE 23
Relevant information
▪ Regional resources: Neurosurgical centre 300 km (185 miles) away
Questions
23.1 Outline your plan for safe patient transfer to and from the radiology department.
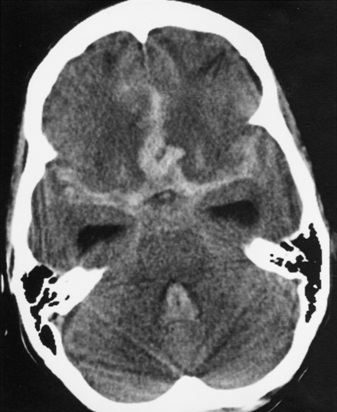 |
Discussion
23.1 Intra-hospital transport of critically ill patients occurs frequently. Transports are usually required to facilitate critical investigations and interventions or to move the patient from one critical-care area (e.g. Emergency Department) to another (e.g. ICU). Critically ill patients with minimal or no physiologic reserve undergoing such transports are at risk of clinical deterioration and adverse events are well reported1.
To minimise potential adverse events, a structured approach for all intrahospital critical-care transports is required. Intrahospital transport guidelines and protocols may vary regionally. A broad outline is detailed below.
Risk–benefit assessment
Patients undergoing invasive ventilation and who require high levels of intensive care support should not be transported for non-urgent interventions or investigations. In this scenario, the need for urgent imaging, potential intervention and ongoing care outside the Emergency Department clearly supports the requirement for patient transport.
Patient stabilisation
• Although acute threats to life have been addressed, a definitive diagnosis is unclear. Further investigation is therefore required before any therapeutic options (if any) are considered. Thus, in this scenario, patient transport for definitive investigation can be considered part of the stabilisation process. Prolonged periods of time in the Emergency Department performing multiple invasive procedures and attempting complete physiologic normalisation are not appropriate.
• Clinical reassessment should occur swiftly, systematically and, whenever possible, with the patient already supported by the equipment that will be used during transport.
• The airway should be checked and secured, endotracheal suction performed, ventilation and oxygenation optimised, adequate and patent vascular access secured and drainage devices measured and emptied. Sedation and analgesic requirements should be addressed and any drugs required for transport (including additional infused agents) pre-drawn and labelled for immediate use.
• Neuroprotective care should be provided, despite the current undifferentiated nature of the presentation (see Case 10). Specifically, hypotension, progressive hypertension, hypoxia and hypercarbia or hypocarbia should be aggressively avoided.
• Ensure that the patient clinical record remains with the team caring for the patient at all times.
Communication and coordination
Team brief
• The assembled team (see below) should reassess the patient’s clinical condition, need for transport and predicted clinical requirements.
• Hospital-based protocols and pre-defined check lists assist significantly and avoid oversight of simple but critical requirements, such as adequate oxygen and available suction for the transport.
Receiving unit(s)
• The initial receiving unit will be the radiology department. Communication should confirm an agreed time for the investigation. This will allow the team to arrive with enough time to transfer the patient safely onto the CT scan machine.
• Following the investigation, consider again the receiving unit, which may vary dependent upon the CT findings. Possibilities include the Emergency Department, the ICU or an operating theatre. All relevant units should therefore be made aware of the pending transport and investigation, as well as the working diagnosis and current clinical plan.
Specialist clinicians
• If not already involved, a senior neurosurgical doctor and radiologist should be contacted.
Transport route(s)
• This should be decided prior to departure. Where possible, the route should avoid common public access areas, lifts and clinically isolated, poorly lit, exposed, narrow (limiting 360 degree patient access) or cramped areas.
Contingency plan(s)
• As a team, consider and verbalise the worst-case scenario. Plan how you will respond should this occur. This may include a plan to move to the nearest appropriate area for resuscitation, which may vary during the journey.
Communication devices
• A fully charged, dedicated and serviceable mobile phone should be carried during the transport. This will be required should there be a need to call for urgent assistance, or in order to facilitate ongoing clinical communication.
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








